No longer neglected
A Zimbabwean clinic’s aim is to vanquish dire ear, nose and throat ailments in children

Peter Koltai, MD, first met 3-year-old Paige Bunjira in May while visiting with a renowned Zimbabwean stone sculptor whose work he admires. Koltai, professor of otolaryngology and of pediatrics at Stanford Medicine, has often visited Zimbabwe as an adviser in the establishment of an ear, nose and throat clinic for children in Harare, the nation’s capital.
This time, Koltai was traveling with his wife, Rita, and they had just purchased a piece from Locardia Ndandarika, one of the country’s first woman sculptors. While sharing tea with Ndandarika, multiple generations of family members joined them, including Paige, who is Ndandarika’s great-granddaughter.
Related Reading
Stanford-Zimbabwe partnerships enable physicians, researchers and students to learn together in Zimbabwe and the United States.
When an aunt realized Koltai’s medical specialty, she told him, “You know, our Paige seems to have lost her voice.”
That got Koltai’s attention. After hearing more, he suspected that Paige had recurrent respiratory papillomatosis, a disease caused by the human papilloma virus, or HPV, which results in small, wartlike growths, typically on the vocal cords — as in Paige’s case.
So he contacted his friend and the man he had aided in setting up the clinic, Clemence Chidziva, MD, a surgeon and professor of otolaryngology at the University of Zimbabwe, who quickly got in touch with the family and arranged the evaluation.
Paige underwent her first procedure to have the growths removed the next month at the pediatric otolaryngology clinic at Harare Children’s Hospital that Chidziva helped open in March 2017. It was the first such clinic in Zimbabwe and only the second in Africa; the first was in neighboring South Africa.




In a country of more than 17 million people, there are only 10 otolaryngologists, also known as ear, nose and throat surgeons. Many consider the subspecialty of pediatric ENT a luxury because of Zimbabwe’s other unmet health care needs. But Chidziva knew the effects of malnutrition, poor medical care and uncontrolled infection on his young ENT patients. He also knew that these problems reached far beyond Zimbabwe into other parts of Africa and the developing world.
Now, thousands of new patients a year make daylong trips by bus to be treated for long-neglected conditions, and the clinic’s founders envision it as a training ground for African otolaryngologists and health care workers who seek to increase their knowledge in the care of these vexing and sometimes serious problems.
“This was a bold dream for a full-scale clinic with audiology and speech therapy services, as well as two operating rooms with a recovery room and beds for overnight care,” said Koltai, whom Chidziva recruited almost five years ago as a volunteer adviser and participant for the project. “Now we believe that this new clinic can be used as a model to be duplicated in other regions of Africa.”
The problem
The children’s hospital is part of Harare Central Hospital, which also includes an adult hospital, maternity hospital and psychiatric hospital. Conditions are difficult. Prior to the opening of the new clinic, Chidziva’s pediatric ENT patients received care at the adult hospital. When Koltai first traveled to Zimbabwe to advise Chidziva, he stayed in the background, listening and learning about the problems he and Chidziva’s staff were going to try to fix.
“I saw the fragility of this medical system,” Koltai said. “The lack of supplies, questionable water and electricity, the marginal cleanliness outside of critical areas in the hospital. There were no fiber-optic capabilities — that is, medical equipment used for internal examination of the body — and no record keeping for patients. But I also saw the dedication of these doctors, who were working under conditions we would find almost intolerable at Stanford.”
The types of ENT problems that Chidziva routinely treated — and that Koltai would eventually assist with during his repeated visits to Harare over subsequent years — were far more serious than the general population understands, Chidziva said. There’s a common misperception in Zimbabwe that ENT problems in children are trivial: Parents think that continually running noses, constant snoring and painful ear infections are just a way of life.
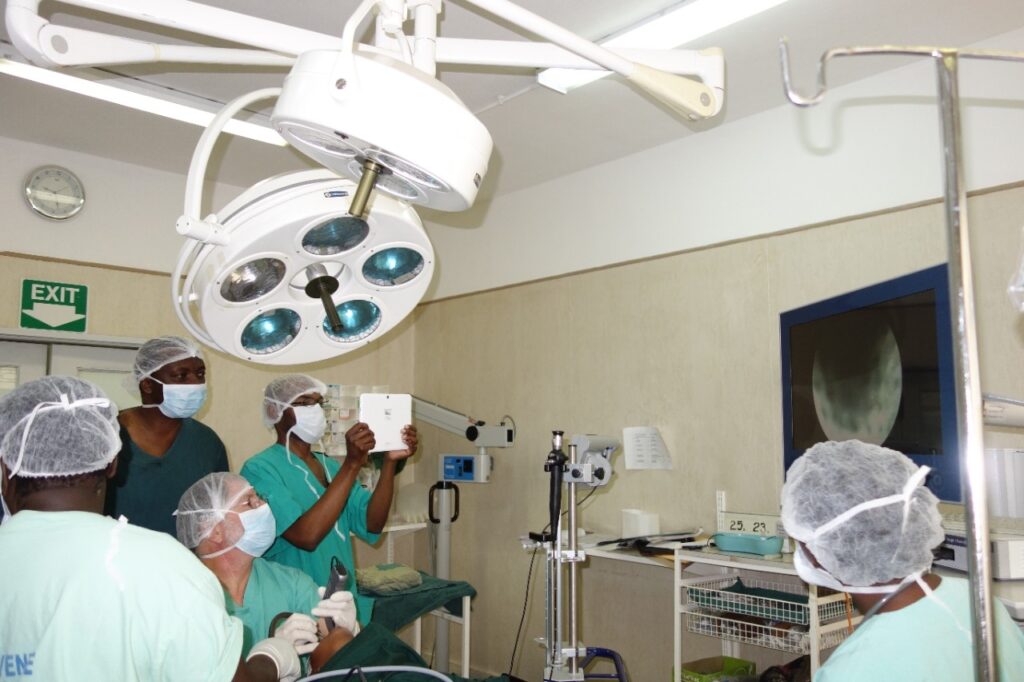
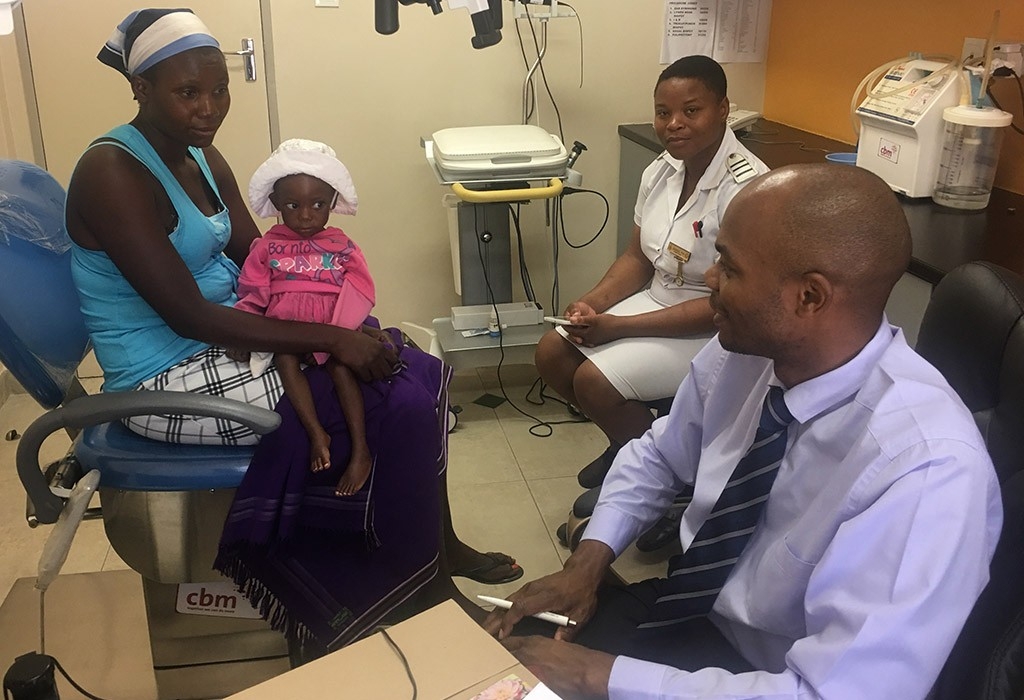
But the list of serious problems is long: tuberculus ear infections with perforated eardrums and often deafness; HIV-associated epiglottitis; obstructed airways; malignant thyroid tumors; congenital neck masses; ingested button-cell batteries; leeches that crawl into the ears of babies left to play in the grass, causing uncontrollable bleeding.
“Many of these things are no longer problems in the modern world, but big problems in the developing world,” said Titus Dzongodza, MD, who was the first graduate of the otolaryngology residency Chidziva started, and the clinic’s initial director. He is now spending an extra year of training in Australia to become certified as a pediatric otolaryngologist. He will be the first pediatric otolaryngologist in Zimbabwe when he returns to lead the clinic in July.
One of the most serious and common medical problems treated by the Zimbabwean physicians is the recurrent respiratory papillomatosis from which Paige suffers. The HPV virus can pass from mothers to babies during pregnancy or childbirth.
The disorder causes growths in the upper respiratory tract that, though not painful, can limit breathing, damage the vocal cords and become life-threatening. The condition is often misdiagnosed in its early stages as asthma, which delays treatment. Children first become hoarse, then lose their voices, as Paige did, and often stop talking altogether. If the growths aren’t removed, they threaten to block respiration completely and the children struggle to breathe.
“By the time they get to us, they can’t sleep, they’re not growing, their breath is raspy and they are struggling to get in air.”
“By the time they get to us, they can’t sleep, they’re not growing, their breath is raspy and they are struggling to get in air,” Dzongodza said. “Usually they’re about 3 years old when they first show up, then they return maybe three to five times for surgery as the warts keep growing back. It’s a challenge for us, especially when much of the equipment we had been using was quite archaic.”
Shortly after the clinic opened, Dzongodza treated an 8-year-old girl who was gasping for breath when she arrived at the clinic, after having traveled all day with her mother by bus from a rural village hundreds of miles away to reach the nearest hospital.
She was rushed into emergency surgery on that spring evening for what would be her eighth procedure to remove the viral warts from her larynx. As a toddler, she was misdiagnosed with asthma and had arrived at the hospital the first time when she was 3, struggling to breathe. This time, though, she was initially seen at the new clinic, with staff better trained to treat children, and had surgery at the children’s hospital with new equipment designed for use with children.
“All the surgeons on the unit had met her one way or the other over the years,” Dzongodza said. “Often, the senior colleagues would dig into their pockets to get her bus fare for the next journey back to the hospital.”
The clinic
To make his vision of starting a clinic a reality, Chidziva started by raising funds for construction from the Christian Blind Mission International, a charity committed to improving conditions of those living in some of the poorest communities in the world. Next, he invited Koltai to join his team. Koltai’s prior experience in establishing the pediatric ENT programs at the Albany Medical College and the Cleveland Clinic, and leading the pediatric otolaryngology program at Stanford as its director for 10 years, proved invaluable, Chidziva said.
“Clemence had a vision, and I bought into it,” Koltai said. “This project resonated with my goals of seeing the footprint of pediatric otolaryngology spread far and wide. I would supply some of the knowledge and know-how, and Clemence supplied the leadership.”
Recognizing the need for specific tools and instruments for a pediatric otolaryngology unit, Koltai has since spent endless hours scanning eBay to scrounge up reusable medical equipment at affordable prices. He shipped two decommissioned surgical microscopes from Lucile Packard Children’s Hospital Stanford to Harare and has been key in plans for the delivery of an ultrasound machine as well as other instruments. The Jenks family of Menlo Park, who had supported Koltai’s research work in the past, helped fund the eBay purchases and shipping costs.
Early on, he secured funding from Stanford’s Department of Otolaryngology-Head and Neck Surgery to fly two senior resident physicians to Stanford for a month of study. This has become an annual observorship with continued funding from the otolaryngology department and accommodations provided by the Koltais in their home. Stanford’s Center for Innovation in Global Health provided seed funding for Koltai’s first trip to Zimbabwe, along with continued financial and moral support.
“Peter’s work, together with his Zimbabwean counterparts’, helping to stock the clinic with instruments and develop a training program for the surgeons, was a terrific example of an equity partnership.”
“Peter’s work, together with his Zimbabwean counterparts’, helping to stock the clinic with instruments and develop a training program for the surgeons, was a terrific example of an equity partnership,” said the center’s director Michele Barry, MD. “Having worked on and off in Zimbabwe for almost 30 years, I can tell you that this accomplishment was no small feat.”
Koltai has returned repeatedly to Harare to teach advanced surgical techniques, hold seminars and set up a record-keeping system for patients in the new clinic. The record keeping will be essential for Chidziva’s long-range plan of creating a training ground at the clinic for future pediatric ENT surgeons, along with a research program to better understand the otolaryngologic needs of African children and develop data suitable for publication to help advance academic appointments at the University of Zimbabwe.
The first research project on the docket, he said, will be a clinical trial to identify the subtypes of HPV responsible for papilomatosis in Zimbabwe.
“We feel that with scientific evidence to support us, we can get our government to change to a vaccine that is effective against the HPV subtypes responsible for this disease,” Chidziva said.
Still, the clinic remains a work in progress. Plans are moving ahead to open an outpatient surgicenter adjacent to the clinic. The surgicenter would have two operating theaters dedicated to treating children with ENT problems. Fundraising has been amped up to fill gaps in care caused by the tripling of the patient load following the opening of the clinic. Constant funding shortfalls mean that much of the equipment considered essential at Stanford, such as MRI or CT machines, remains out of reach in Harare.
“When we created this clinic, we did it to improve care for our patients,” Chidziva said. “But within the first year of opening, we saw 3,500 patients, three times the average caseload. The struggle now continues to get them all onto an operating table in time.”
The future
Last May, the team organized the first international symposium to advance pediatric otolaryngology to be held in Africa.
Called PENTAfrica and held in Zimbabwe, it was attended by otolaryngologists and other health care professionals from Africa, Europe, and North and South America. The event launched the organizers’ plan to use the children’s clinic as a model to provide education, expertise and greater access to care across the continent.
“We’re hoping our new clinic will plant a seed in each and every country in Africa,” said Chidziva. After Dzongodza returns from Australia, fully trained in pediatric otolaryngology, and the clinic’s operating wings open in July, Chidziva plans to invite ENTs to observe Dzongodza in his work so they can better understand the needs of pediatric patients and how they might be able to replicate the clinic’s model.
“We’re hoping our new clinic will plant a seed in each and every country in Africa.”
Still, such immediate needs as tracking down equipment and even navigating for hospital space for surgeries continue to challenge their ability to ensure treatment for children like Paige. The virus is especially aggressive in young children, including Paige, who needed a second surgery in November and a third in December. Then, a 40-day doctors’ strike left the clinic’s senior registrar, Erasmas Muganda, scrambling for two days — amid a flurry of communications with Chidziva and Koltai — to find a space to operate.
Koltai said he will do what he can to help the clinic build capacity to treat children like Paige, and he marvels at how his connection with the art of sculpture brought her into the clinic’s fold. A lifelong artist, Koltai provides medical illustrations for his own publications and recently began formal training in painting.
“What inspires me about Paige is how serendipity has tied together my work in both the medical as well as the sculpture communities,” Koltai said. “My life’s work has revolved around taking care of kids and making art; the yin and yang of my being. Somehow this story has the scent of fate.”

