No limit?
Challenging the view of sickle cell trait
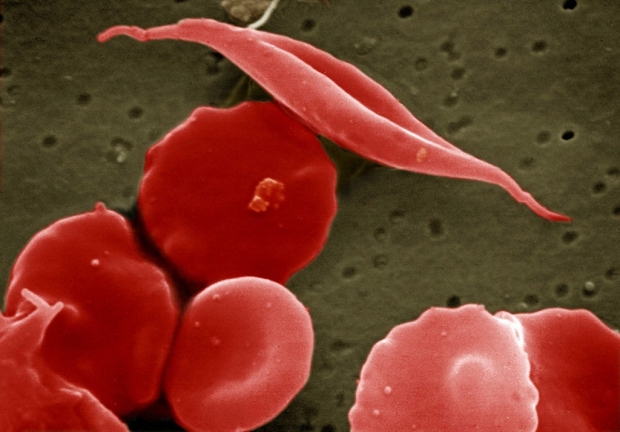
If you inherit a sickle cell gene variant from each of your parents, the result is sickle cell disease, which in its most severe form leads to bouts of intense pain and can drastically shorten your life. But what if you carry just one copy of the sickle cell variant — as is the case for 1 in 13 African-Americans?
Earlier studies had suggested that this status, known as sickle cell trait, could have dire consequences, including higher mortality from a condition called exertional rhabdomyolysis, which has been known to fell football players, often when they are practicing too hard in the hot sun without drinking enough water. ER, which occurs when molecules from the breakdown of muscles end up in the kidneys, is also a risk for soldiers on active duty.
But Stanford associate professor of medicine Lianne Kurina, PhD, questioned these studies. When she reviewed the literature, she saw it was dominated by reports about individual patients. She also saw that in one influential study — from a large population — the actual sickle cell trait status of every individual was not known.
In search of a more definitive answer, Kurina and her colleagues conducted the first-ever longitudinal cohort study of sickle cell trait in African-American soldiers of all ages. The result: no increase in mortality for soldiers with sickle cell trait, provided they follow standard safety precautions, including gradual increases in exercise and adequate water and rest breaks.
For the study, the researchers reviewed the health records of 47,944 African-American soldiers who served on active duty between 2011 and 2014 and for whom sickle cell status was known. The researchers got the health records from the Stanford Military Data Repository data set, which was created by Kurina and D. Alan Nelson, PhD, a postdoctoral scholar and former Army medical officer.
The repository includes all digitally recorded health encounters at military medical facilities or civilian institutions, general health information, and official records of physical performance and mortality of all active-duty U.S. Army soldiers. To protect privacy, the data in the repository are de-identified.
The researchers found that the risk of exertional rhabdomyolysis was only 54 percent higher among African-American soldiers with sickle cell trait than among those without it. A 54 percent increase might sound like a lot, but it’s far less than the 300 percent increase caused by some ordinary prescription drugs. And smoking, obesity and increasing age each incurs a heightened risk of ER that is about the same as sickle cell trait’s, the study showed.
“The most important thing to come out of this study is the really reassuring news that under conditions of universal precautions against dehydration and overheating, we don’t see an elevation in the risk of mortality in people with sickle cell trait,” says Kurina.
The assumption that sickle cell trait increases health hazards has led to mandated screening by organizations such as the Air Force, the Navy and the NCAA. But the American Society of Hematology and other organizations have argued that screening programs raise questions about job discrimination.
The study’s results call into question the need to screen service members with sickle cell trait, especially with better safety precautions during intense exertion, Kurina says.
Kurina, Nelson and their team published the study in August in The New England Journal of Medicine.

