Beyond the bench
Surprising and sometimes strange biology fuels the future of medicine

Hundreds of Stanford scientists are on a quest to understand what makes biology tick — from obscure molecular structures in the malaria parasite to flower-shaped sea squirts that teach us about our own immune system.
In this roundup of basic biology research, protein-producing organelles, tadpole tails and flesh-ravaging parasites take center stage, exemplifying some of the curiosity-driven science at Stanford Medicine that might one day come to bear on human health.
Imagine being fused to your closest relatives and, try as you might, there’s no chance of untethering. Such is the life of the sea squirt, Botryllus schlosseri.
The biology of these ocean denizens, which as a colony look almost like aquatic daisies, has some uncanny similarities to that of humans. Irving Weissman, MD, director of the Stanford Institute for Stem Cell Biology and Regenerative Medicine, has studied these animals for decades, investigating the role that genetics and stem cells play in their survival.
The sea squirts Weissman studies live in colonies enveloped by a shared outer translucent sheath, called a tunic, and every flowerlike colony is physically unified by a single blood vessel that threads through each petal-shaped sea squirt.
“These blood vessels have a very funny nature to them. They not only connect through the individual animals, but at the edge of the tunic they have an end that protrudes out, like a little balloon,” explained Weissman.

The vessel acts a recruiter of sorts. Sea squirts, which glom onto rocks and other hard surfaces below the tide, can reproduce asexually, expanding their colony by creating new buds composed of stem cells. There is, however, a quicker way to grow. Before sea squirts begin to form colonies, they compete for subtidal real estate and often settle in the same general region.
As two colonies expand, nearing one another, the blood vessel from one sea squirt juts out and pokes into its neighbor. The immune cells contained in the appendage then administer a sort of pass-fail genetic test: Only sea squirts with specific genetic overlap will be accepted into the group.
“If the genetics match up, individual sea squirts from the probing colony send out blood vessels to infiltrate the tunic of the new colony, hooking up their vasculature to all of the new individuals,” said Weissman.
The two colonies join their blood circuitry, allowing floating stem cells to pass from one colony to the other. In a pair of merging sea squirts, there’s often one that’s genetically dominant, taking over the gonads (which produce eggs or sperm) of both colonies. After some time, the eggs or sperm of the dominant sea squirt assert themselves as the genetic template for future offspring.
On the flip side, if the probing blood vessel deems the new sea squirts too genetically foreign, the probe is literally scarred, unable to form any future blood bond with another colony. Weissman’s research has pinpointed a single gene, bhf, that arbitrates fusion or rejection.
“If the genetics match up, individual sea squirts from the probing colony send out blood vessels to infiltrate the tunic of the new colony, hooking up their vasculature to all of the new individuals.”
Irving Weissman, MD, director of the Stanford Institute for Stem Cell Biology and Regenerative Medicine
Sea squirt immune cells can tell if a potential colony mate has a bhf gene that aligns with its own biology. If the genetics don’t match up, immune cells in the outstretched blood vessel kill off the external cells with which it came into contact, rejecting any potential fusion. Only kin that share a bhf gene can unite via blood vessel.
The discovery adds to an earlier finding of Weissman’s group that suggested this invertebrate sea squirt harbors blood-related genes and killer immune cells that, surprisingly, resemble those found in vertebrates.
It may even provide insight into how the human immune system distinguishes self from other, similar to what happens after bone marrow transplants. The unexpected common ground has fueled a push, pioneered by Weissman and former trainees, to harness Botryllus schlosseri as a new model organism to study immune biology.
Furthermore, Weissman said, the stem cell competition that allows one sea squirt to genetically overthrow another, which was discovered by Weissman’s group in the 1990s, made him wonder if blood stem cells might compete with each other in a similar way, and if that could play a role in aging and the development of cancers.
His team later demonstrated that this was the case and that human blood stem cells can acquire mutations that make them dominant over other normally functioning blood stem cells. The finding has already started to map out how faulty human stem cells can snowball into diseases like leukemia, a cancer that affects bone marrow.
The tail end
There aren’t many animals that can sprout an entirely new appendage with flawless precision. For a week of its early life, the western clawed frog, Xenopus tropicalis, is one of the lucky few.
During this brief window, the fledgling amphibian possesses the extraordinary ability to replace its own tail, should it find itself in a pinch. If its southmost appendage is somehow lost, the tadpole grows a replacement within a week — including its spinal cord, veins, muscle and the outer tadpole skin.
That’s a lot of molecular coordination, and it’s something that Julie Baker, PhD, professor of genetics, studies in her lab at Stanford. Her focus: the molecules and genes that allow these tadpoles to restore their rears, focusing on the initial steps of the regeneration process.
To understand what happens during tail regrowth, Baker and her team looked at samples of tadpole RNA — a molecular cousin of DNA that acts as a template for proteins — during several time points while a tadpole was undergoing regeneration.
With the RNA data as a guide, several genes emerged as possible regulators of the process. Using CRISPR-Cas9 gene editing technology, Baker’s lab inhibited the suspicious genes’ functions one by one, singling out those that were needed for full tail regeneration.
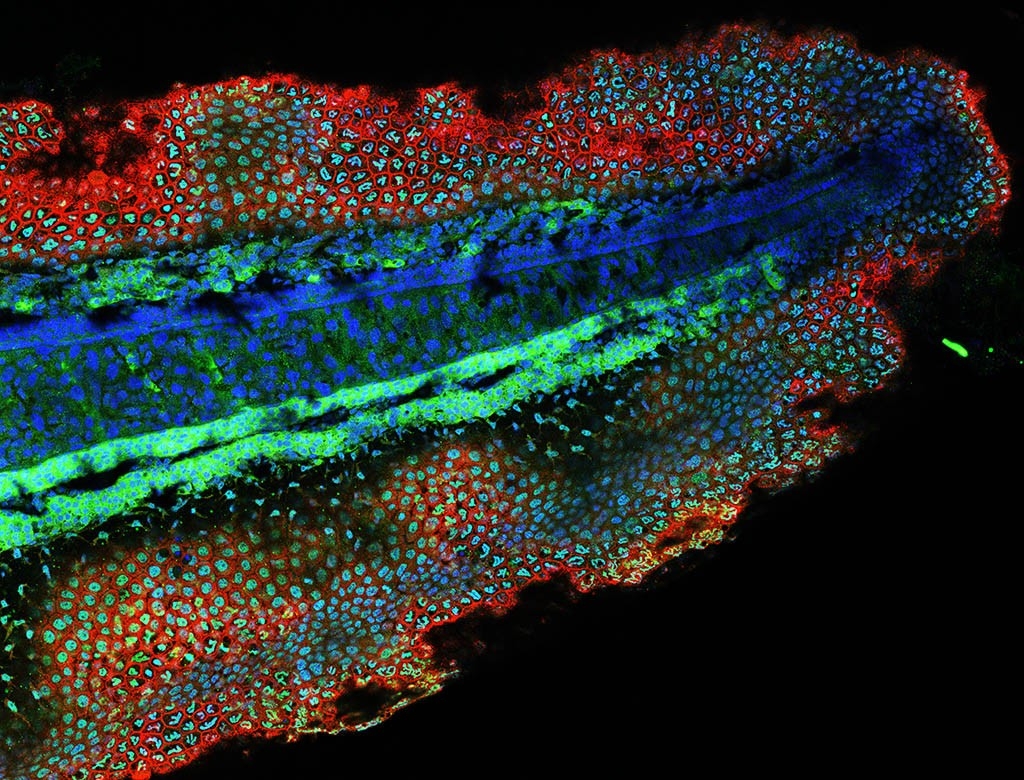
They then turned to microscopy, and what they saw was equally intriguing. All animal cells contain a nucleus that encases and protects DNA. Under normal conditions in a tadpole, the cells near the outermost layer of the tail have nuclei with wonky, haphazard shapes, or as Baker described them, shapes that “look like alphabet soup.” In other tissues, the tadpole cells contain spherical nuclei. When the tail is lost, something curious happens.
“The cells with the alphabet-souplike nuclei change; some start to move away from the site of injury, and some start to morph into the spherical nuclei,” Baker said. The result is a swarm of cells with spherical nuclei at the site of tail loss. Three hours later, like clockwork, the cells with wonky nuclei return, some moving physically back to their original location, others forming when spherical nuclei morph into wonky ones.
“The thing about regeneration is it happens really differently in different organisms: Zebrafish can regrow their fins, and axolotl salamanders can regrow limbs, but the processes don’t look the same molecularly.”
Julie Baker, PhD, professor of genetics
And then another three hours pass, and the nuclei flip back to the spherical form. What’s more, if the cells are prevented from executing their flip-flopping routine, regeneration ceases. “It’s like these changing nuclei are really guiding this process,” said Baker. “There’s something very strange about that, but it’s also very exciting.”
Now, Baker and researchers in her lab are examining the shape-shifting process, aiming to better grasp the genetic drivers that imbue the tadpole with regenerative power, and how those drivers relate to the changing shapes of the nuclei. It’s possible, Baker said, that the form a nucleus takes influences which genes are turned on by altering which of them are accessible to molecules that flip the switch.
While the squiggles of tadpole nuclei don’t necessarily hold the secret to human limb regeneration, Baker sees the research as informative for wound healing and spinal cord generation for more than just frogs. After all, the majority of the animal kingdom shares a common biological lineage, so lessons from one could apply to many.
“The thing about regeneration is it happens really differently in different organisms: Zebrafish can regrow their fins, and axolotl salamanders can regrow limbs, but the processes don’t look the same molecularly,” Baker said. “Knowing more about how various species regenerate under different contexts will give us more of a total picture about what’s possible in biology.”
The one-organelle wonder
Inside the Plasmodium parasite, which causes roughly 500 million annual cases of malaria, is an oddly shaped molecular structure that keeps it alive: the apicoplast. This obscure organelle, found only in a small class of single-celled parasites, is a key driver behind malaria’s deadly pathology.
“If you think of organs in the human body as having special roles — the heart pumps blood, the kidneys clear toxins and so on — organelles are like the cellular versions of that,” said Ellen Yeh, MD, PhD, assistant professor of biochemistry, of pathology, and of microbiology and immunology who studies the ins and outs of the apicoplast. “They’re these little machines in the cells that each have a dedicated role.”
Yeh’s past research found that a key product of the apicoplast is isopentenyl pyrophosphate. In and of itself, IPP possesses no special powers; it’s a common base material for other molecules that are important for the parasite’s survival. “I think of IPP as the brick in a building: It’s a starting material or building block that can be used to build lots of different types of structures with different purposes,” said Yeh.
She suspects that IPP could play a handful of roles in the cell, such as signaling or shuttling other molecules around. Yeh and her lab are trying to identify how IPP works and in what context so they can use the information to develop an anti-malarial drug. The scientists’ quest couldn’t be more timely: The only existing malaria treatment faces challenges because drug-resistant strains of Plasmodium are beginning to crop up.
“If you think of organs in the human body as having special roles — the heart pumps blood, the kidneys clear toxins and so on — organelles are like the cellular versions of that. They’re these little machines in the cells that each have a dedicated role.”
Ellen Yeh, MD, PhD, assistant professor of biochemistry, of pathology, and of microbiology and immunology
But at the end of the day, much of the anti-malaria efforts come back to the apicoplast. Every stage of the Plasmodium life cycle — during which the parasite infiltrates a human host by way of a mosquito bite, replicates in the liver and then spreads through the blood — depends on the apicoplast.
“We don’t know if IPP is required during every stage of life for the parasite,” said Yeh. But we know that the apicoplast, which makes IPP, must be present in all living malaria parasites — if it fails to form when the Plasmodium reproduces, the parasite simply dies.
Now, researchers in her lab are on the hunt for genes that regulate apicoplast formation. The idea is to identify genes that are indispensable to apicoplast formation during Plasmodium development and tweak those genes to halt the parasite’s life cycle.
“We’ve already found two enzymes that are required for apicoplast formation, so instead of working to get rid of the individual IPP molecules, we’re basically working to blow up the factory,” said Yeh. “It’s scary and exciting at the same time because we don’t know what the mechanism is, but we can see the end result of eliminating these enzymes. We see that the apicoplast is gone and that the cell can’t survive; now we just need to figure out how that happens.”
Out for blood
Parasitic worms known as schistosomes lurk in the freshwater rivers, streams and lakes of tropical and sub-tropical regions, waiting to bore into a host. The stealthy intruder, commonly known as a blood fluke, is a tiny, canoe-shaped stowaway that manifests as a disease called schistosomiasis in humans, triggering itchy rashes, malnutrition and, in the worst cases, organ failure.
Bo Wang, PhD, assistant professor of bioengineering, studies the life cycle of the schistosome parasite, investigating the genes and stem cells that allow the voracious worm to invade its host.
The creature’s yearning for human flesh is prepped by a series of morphological changes throughout its multistage life cycle. It starts in water, where it hatches from an egg, taking on a “teddy bear-looking” physique — fuzzy and plump — while seeking out aquatic snails.
Once inside a snail host, the parasite, about a tenth of a millimeter long, morphs into a sac of stem cells and multiplies to boost its numbers.
“It’s sort of a Russian nesting doll situation,” Wang said. “Hundreds of thousands of new parasites are born from a single invasion until the snail is just kind of a zombie overrun by schistosomes.”
The blood flukes hunker down in their snail host until signals of an accommodating environment — more light and warmer temperatures — coax them from their temporary keeper.
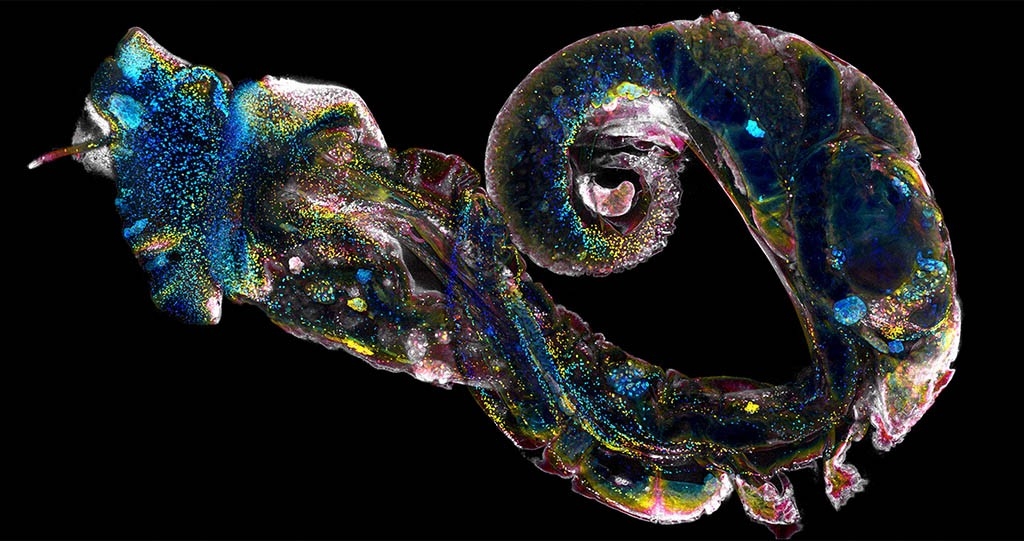
During this transition, the blood flukes change form again to adapt to a watery environment, and they emerge from the snail looking like a cross between a tadpole and a bullet. The long, pointy morphology not only helps the flukes flit through water, it also allows them to burrow through human flesh.
Once they’ve tunneled in, they take a very specific course. First, they head to the lungs, where they start to morph into yet another form. From the lungs, they navigate to the liver, where they become sexually mature worms.
At this stage, however, the sheer presence of the blood flukes isn’t an issue for humans. It’s what happens next that’s problematic.
“Each female can lay thousands of eggs every day, and she can do it for decades,” said Wang.
Massive numbers of eggs eventually clog the human body’s blood vessels and become lodged in organs, causing the immune system to rev up its inflammatory response. Left untreated, the immense egg deposit can cause tissue scarring and fatal organ failure.
A drug treatment exists for schistosomiasis, but it’s not very effective. The drug knocks out only the full-grown blood flukes, so any immature worms present still grow up into adults that can make more eggs. In many cases, the infection returns even after a patient is treated.
“Each female can lay thousands of eggs every day, and she can do it for decades.”
Bo Wang, PhD, assistant professor of bioengineering
What’s missing is a way to eradicate worms at all stages simultaneously, or a way to stop the parasites from growing into sexual maturity in the first place.
“We’ve been dissecting cells and parsing their genetic information, specifically looking at how stem cells play into the transitions from one body shape to the next,” said Wang.
Through molecular sequencing techniques, Wang discovered that the activity of one gene in particular, eledeh, seems to set maturation in motion inside the human host.
“It’s basically the initial switch. Once the worm infects the human, eledeh signals allow the worm to start developing the subsequent, sexually reproductive-friendly form.”
Dissecting the inner workings of blood flukes is not only fascinating, it’s turning up clues for drug development, said Wang. A drug that knocks out eledeh could be devastating for the worms yet would probably be harmless to humans because there’s no human version of eledeh.
But before Wang thinks about pursuing therapeutics, he wants to work out more of the biology to clear up what eledeh controls and how the blood flukes fare when the gene is tampered with.
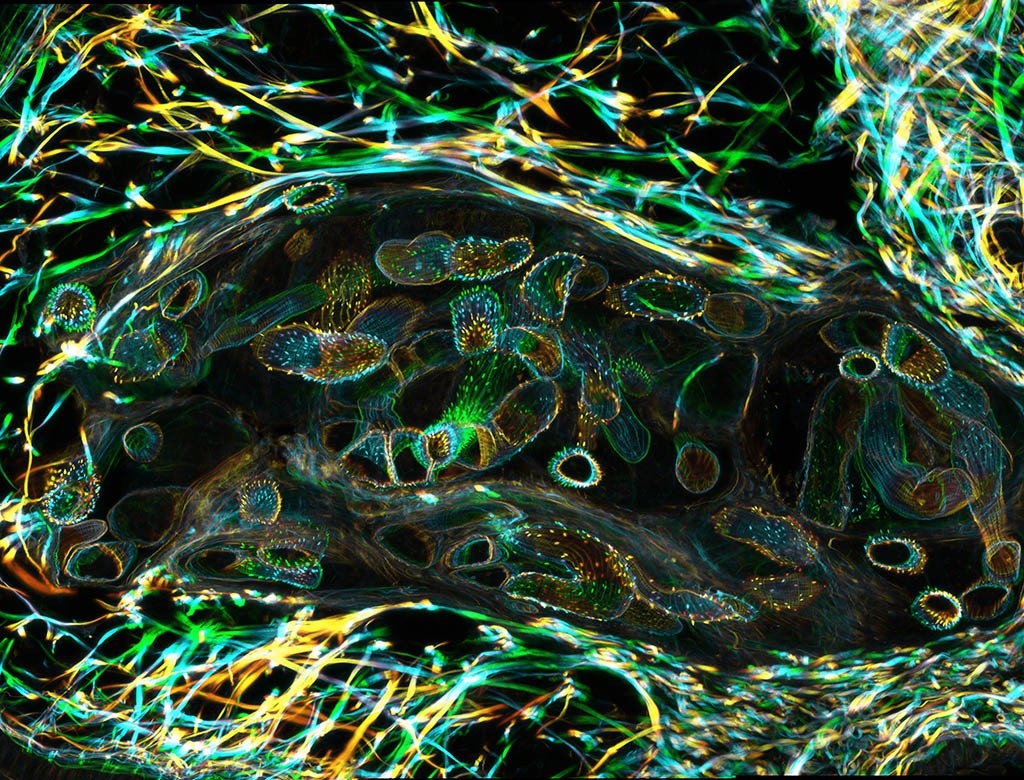
The picky ribosome
Inside every cell, millions of molecular machines called ribosomes diligently churn out proteins, the workhorses of the body.
Decades of ribosome research has yielded a reliable understanding of the protein manufacturing process: Snippets of genetic information, known as messenger RNA, float freely in a cell until they bump into one of the many ribosomes.
Upon contact, the ribosome pulls a piece of genetic code into its machinery and, as if knitting a sweater from unspooled yarn, assembles the protein. It’s estimated that the human body can make millions of different proteins.
Until recently, biologists thought any ribosome could synthesize any protein type. But two years ago, Maria Barna, PhD, assistant professor of genetics and of developmental biology, discovered these microscopic machines have some say in what proteins they make.
Special molecules embedded in ribosomes act like gatekeepers, accepting some mRNAs and shooing away others. Depending on the class of gatekeeper molecule, the overall configuration of the ribosome changes.
Barna suspects that the modifications in ribosome composition may contribute to a lock-and-key mode of operation, in which the subtle structural specificities of a ribosome determine which mRNAs are welcomed for protein production.
What’s more, these gatekeeper molecules actually track with biological categories of mRNA. For example, some ribosomes accept only mRNA that carries the code for proteins involved in embryonic development; others, only mRNA for certain metabolic pathways.
It looks like there may even be a hair ribosome, which selectively processes mRNA that codes for hair proteins — specifically, hair on the face and scalp.
“My favorite example is one that involves a ribosome with an embedded protein called ribosomal protein SA. If that protein is missing, the only resulting effect is a loss of the spleen. Everything else seems absolutely normal — it’s pretty wild.”
Maria Barna, PhD, assistant professor of genetics and of developmental biology
“But my favorite example is one that involves a ribosome with an embedded protein called ribosomal protein SA,” Barna said. “If that protein is missing, the only resulting effect is a loss of the spleen. Everything else seems absolutely normal — it’s pretty wild.”
Gone was the notion that ribosomes are protein-making drones. Instead, Barna’s finding was the first to frame ribosomes as choosy genetic regulators, capable of exercising discretion with incoming mRNA.
“These are some of the first examples in which ribosomes show their potential power in gene regulation,” said Barna. “This finding shows that the ribosome may be critical to the diversity of proteins that can be expressed within a cell, within a tissue or within organisms.”
It is still unknown exactly how many ribosomal classes exist. Barna said that she and researchers in her lab have identified dozens of differences in ribosome composition.
For example, in a eukaryote, 80 different core proteins can glom together in multiple ways to make a ribosome, but every ribosome does not necessarily contain the same proportion of core proteins. So one ribosome could include one or more of a particular core protein, while its neighbor might not have that protein whatsoever.
It’s essentially a numbers game: With this type of variation possible for 80 different proteins, Barna said, there could be hundreds of thousands of different ribosome configurations out there. “But until we can track ribosomes across all cell types, which we’re working on right now, we won’t have a definitive answer.”
The realization that core components of ribosomes are mutated in a variety of human diseases opens up the possibility of manipulating ribosomal discretion for therapeutic purposes. It’s an idea that’s theoretically ripe with potential, but Barna cautions that the research is still early. Whether ribosomes can be used against disease is still a question mark.

