A better way to resuscitate
Stanford-India biodesign fellows invent a device that helps newborns breathe on their own
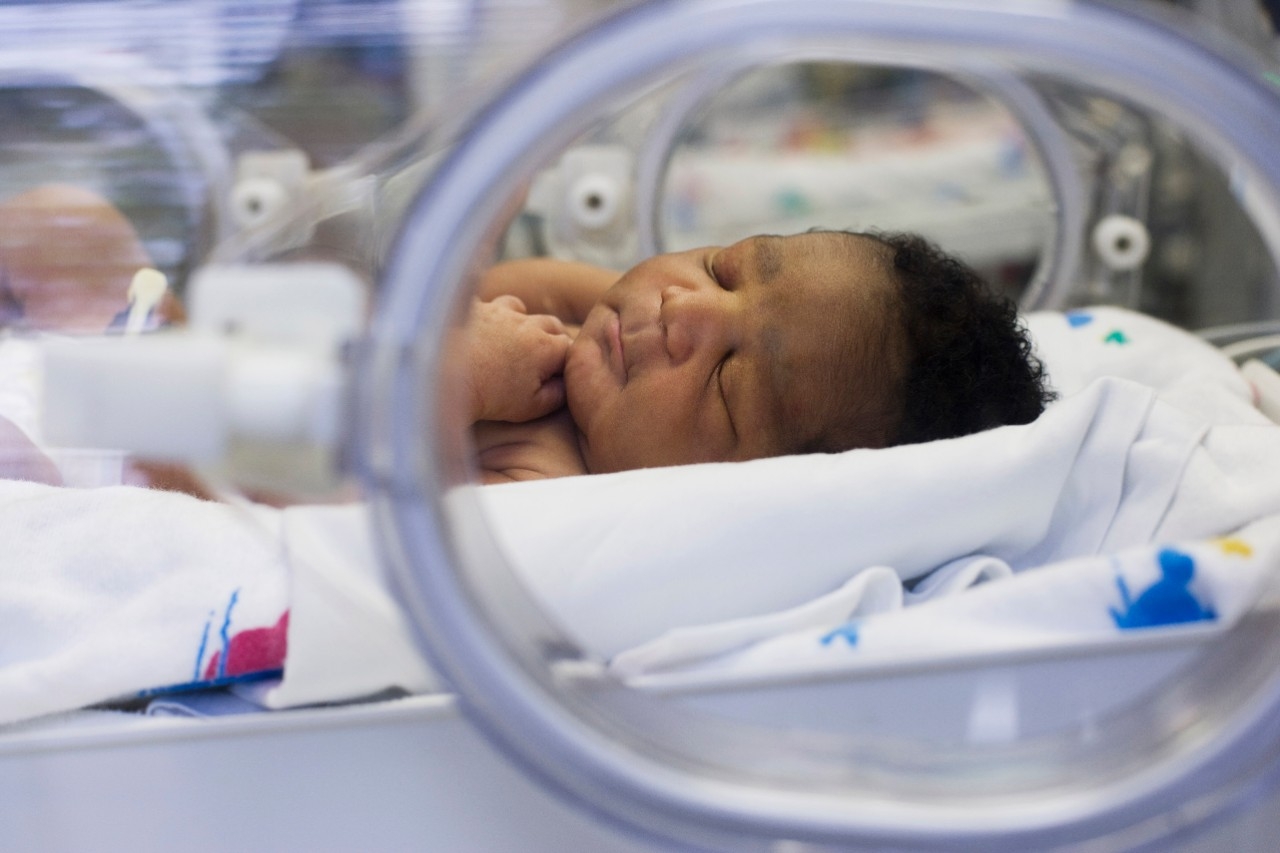
In the United States, resuscitating a baby who suffers from birth asphyxia is relatively simple. When a newborn fails to breathe, one clinician holds a respirator mask to the baby’s face while another person squeezes a ventilation bag, pushing air into the baby’s lungs.
But in low- and middle-income countries such as India, where staff is more limited, resuscitation is not so straightforward. An individual clinician commonly resuscitates the baby alone, using one hand to perform a triple maneuver of a jaw thrust, chin lift and neck tilt, sealing the respirator mask around the baby’s mouth, and using the other hand to squeeze the bag.
According to the World Health Organization, birth asphyxia causes about a quarter of the 2.5 million newborn deaths each year.
“In the absence of adequate training, much of the air during resuscitation may leak out, causing the baby to suffocate,” said Avijit Bansal, MD, a pulmonologist from India.
Recognizing a problem, in 2012 Bansal and biomedical engineer Ayesha Chaudhary, PhD, co-founded Windmill Health, a medical device company in New Delhi. They developed NeoBreathe, a foot-operated resuscitator that frees one of the operator’s hands, cuts down on air leakage and significantly improves ventilation. With the freed hand, the operator can multitask more efficiently in that first life-saving minute of a baby’s life.
The idea for the device was sparked in 2011, when Bansal and Chaudhary met through a Stanford Byers Center for Biodesign Stanford-India fellowship and realized they both wanted to improve the treatment of birth asphyxia. Founded in 2000, the Stanford biodesign center aims to provide knowledge, skills and mentoring for people seeking to become health technology innovators.
Through the program, four fellows from India spent six months at Stanford University, studying biodesign innovation and working on team projects, and six months at the All India Institute of Medical Science in New Delhi, zeroing in on unmet health care problems and developing new technologies to solve them.
The fellowship gave Bansal and Chaudhary the skills to design and develop their device. After extensive feedback from product users, several design cycles and thorough testing, the machine was commercially launched in December 2016. The device is now being used in 20 out of the 36 states in India, as well as in Kenya, South Africa, Nigeria and Mali.
Other technologies that have come out of Stanford Biodesign’s India program include Sohum, an affordable device used to screen newborns for hearing defects, and HiCARE LIMO, a cardboard splint that helps caregivers temporarily immobilize injured limbs.
The company plans to introduce NeoBreathe in other countries that need it, including Peru, Chile and Argentina, said Bansal.
“We have created a new way of performing an age-old procedure. It is helping save lives, and people are taking notice,” said Bansal. “This is just the beginning for us.”

