Burnout in brain city
When nerve cells’ power packs go wrong
Advanced life is largely a success story of a tiny bacterium that knew a trick or two cutting a deal, over a billion years ago, with a larger cell capable of safely housing the wee magician.
This was the deal: In exchange for a plentiful supply of oxygen, plus carbohydrates or fats, the bacterial boarder would transform these raw materials into energy the larger cell could use pretty much any way it wanted to.
This magic trick is the process we call respiration. Over time, the once free-living bacterium thrived and evolved to become the subcellular components, or organelles, we know as mitochondria. Mitochondria and the cells in which they dwell have been locked in a symbiotic embrace ever since.
There is a catch, though. The harder a cell has to work, the more energy its mitochondria have to churn out — and the more likely they’ll burn out. Just ask a nerve cell. Or, better, ask a couple of Stanford scientists who have tied mitochondrial morbidity to neurological diseases and used that insight to make inroads in treating Alzheimer’s, Parkinson’s and more.
The dark side of the deal
The downside of respiration is that it inevitably generates nasty byproducts called free radicals, which not only are harmful to the mitochondria but can also damage cells generally — not to mention deprive them of the energy they need to function properly. T
hat cell damage, in turn, can set off a cell-suicide program called apoptosis. When things go wrong with mitochondria, they cough out far larger amounts of free radicals, and then things can go very wrong with us, too.
As free-radical damage takes its toll, battered mitochondria accumulate and overall mitochondrial function declines. While this happens throughout our bodies, some tissues get hit harder than others. The higher a cell’s energy requirement, the more damage you might expect it to incur from the toxic exhaust of mitochondria in overdrive.
With this in mind, consider that about 20% of all the energy our mitochondria produce is used up by our massive, ever-busy brains. The roughly 100 billion nerve cells, or neurons, in the human brain contain hundreds to thousands of mitochondria apiece to generate that energy.
With people living longer, age-related neurodegenerative disorders are more prevalent. The most common member of this club of undesirables, Alzheimer’s disease, affects well over 5 million adults in the United States, with an estimated global prevalence above 50 million.
Parkinson’s disease is in second place, with 10 million people affected. Huntington’s disease and amyotrophic lateral sclerosis — or ALS — are more rare, but are also tragically debilitating.
Each of these disorders is associated with the buildup in the brain of one or another protein that’s toxic to neurons. Neuroscientists and drug developers intent on finding cures have focused their attention on neurons and those neurotoxic proteins. But those considerable efforts haven’t yielded drugs that stop the relentless progression of neurodegenerative diseases.
As free-radical damage takes its toll, battered mitochondria accumulate and overall mitochondrial function declines. While this happens throughout our bodies, some tissues get hit harder than others.
Meanwhile, researchers increasingly suspect mitochondrial mishaps are a driving force behind many neurodegenerative diseases — suspicions strongly confirmed in recently published studies by Stanford scientists. These insights stand to accelerate the rethinking of approaches that haven’t been successful and speed a shift toward stamping out mitochondrial malfeasance. At least two promising drug candidates discovered at Stanford aim straight at mitochondria.
Xinnan Wang, MD, PhD, has been on the trail of Parkinson’s disease for several years. Her discoveries about mitochondria’s role in Parkinson’s are raising hopes that it can be caught before symptoms develop and, perhaps, arrested as soon as the disease is diagnosed.
Whereas 5% to 10% of Parkinson’s cases are familial — the inherited result of known genetic mutations — the vast majority are sporadic, involving complex interactions of multiple unknown genes and environmental factors.
Parkinson’s stems from the mysterious die-off of a set of especially hard-working midbrain neurons that fine-tune our every bodily movement. These neurons are referred to as dopaminergic because a substance they secrete, dopamine, transmits motion-modulating signals to other neurons. By the time a person manifests symptoms, an estimated 50% of these midbrain dopaminergic neurons have already died.
Why these particular cells, and not others, would die is unknown. One leading theory holds that the special intensity with which midbrain dopaminergic neurons perform their duties frazzles their mitochondria.
“Some cells in the body have a soft desk job,” said Wang, an associate professor of neurosurgery. “But these fine-motor-control neurons are working 24/7.”
No Parkinson’s treatment in current use stops those neurons from dying, Wang said.
There also hasn’t been any good way to detect Parkinson’s disease early in its progression. “Early clinical diagnosis is entirely based on observing symptoms and querying patients,” said Wang. The rate of misdiagnosis is about 10% to 20%, she said.
Absent any reliable early marker, drug developers can’t test potential treatments when they might help the most — before patients are symptomatic.
They’re working in the dark, Wang says. “But our new study may provide them with eyes.”
Mitochondria on the move
To do this, Wang’s group focused on how mitochondria move within a cell. You might imagine that, like power plants, mitochondria wouldn’t move much. But they’re frequently shuttled from one part of a cell to another in response to the cell’s internal energy needs.
“Mitochondria are very dynamic,” Wang said. “Between 30% and 60% of them are on the move at any one time.”
Not that they glide around the way their rustic, puddle-paddling, blown-by-the-breeze bacterial ancestors did. In fact, mitochondria’s movements are quite orderly. But they don’t travel on their own. Instead, they spend much of their time attached to a grid of molecular tracks that crisscross cells like elaborate urban-transit tracks, and along which they get hauled like cargo when need be.
Here’s where mitochondria’s hostile work environment (their own selves, that is) comes into the Parkinson’s picture. Defective mitochondria have to be hustled off to cells’ in-house dumpsters as soon as possible, lest their toxic output spur cell damage or death.
For this purpose, our cells have a set of specialized proteins that yank them off the grid to be perp-walked to the cell’s recycling centers. First, though, those proteins have to remove an adaptor molecule called Miro that staples mitochondria, whether damaged or healthy, to the grid.
Wang’s group has pinpointed a cellular defect that stymies those “yanking” proteins’ ability to shave Miro off damaged mitochondria. In a more recent study, published in Cell Metabolism in September 2019, the group found that cells from the great majority of people with Parkinson’s and relatives considered at heightened risk for the condition had this same defect — unlike the cells of anybody else the scientists studied.
Using software belonging to Atomwise, a San Francisco-based biotechnology company, the investigators screened nearly 7 million drug candidates to identify compounds likely to facilitate Parkinsonian cells’ ability to clear Miro from damaged mitochondria and expunge them. They identified a set of 11 compounds, which were also likely to be nontoxic, could be taken orally and could cross the blood-brain barrier.
Researchers tested the most promising compound, which appeared to target Miro almost exclusively, on Parkinsonian cells. It substantially improved these cells’ ability to clear Miro after their exposure to mitochondria-damaging stress.
But these cells were skin cells, and Wang was interested in what this compound would do for neurons. So her team generated dopaminergic neurons from Parkinson’s patients’ cells, incubated them with the experimental compound, and found that these neurons rivaled healthy individuals’ neurons in their ability to scrape Miro from damaged mitochondria and get rid of them.
To further test the compound, the scientists fed it to fruit flies engineered to develop the equivalent of Parkinson’s. Fruit flies and people — whose ancestors diverged from some undoubtedly weird-looking common predecessor about 782.7 million years ago — share many similarities.
The midbrain dopaminergic circuit that controls muscular movement works much the same in them as it does in us. Giving the compound to those flies throughout their 90-day lifetimes prevented their dopaminergic neurons’ deaths and improved their climbing ability, without toxicity signs.
“We’re closing in on a drug that, instead of just providing symptomatic relief, might be able to address Parkinson’s disease’s cause and alter its course,” said Wang. “We believe it could be a major step toward a cure.”
Wang, who formed a company called CuraX to put her team’s findings to work, said she thinks clinical trials of the compound or a close analog are no more than a few years off.
“Miro is a brand-new drug target — pharmaceutical companies haven’t aimed at it before,” she said. “Our hope is that if this compound or a similar one proves nontoxic and efficacious so we can give it repeatedly, like a statin drug, to people who’ve tested positive for the Miro-removal defect but don’t yet have Parkinson’s symptoms, they’ll never get it.”
Halting disease progression
Meanwhile, tantalizing evidence gathered by Daria Mochly-Rosen’s group suggests that several neurodegenerative disorders — including Alzheimer’s, Huntington’s and ALS — are marked by identical inflammatory interactions among a few types of brain cells.
Those interactions employ malfunctioning mitochondria as messengers of death: They travel from cell to cell, emitting inflammatory signals in the form of the toxic free radicals. And their mortal message can be countered by the sustained systemic administration of a substance engineered in Mochly-Rosen’s lab.
“We’ve identified a potential new way to prevent death of neurons in several diseases, regardless of their differing original causes,” said Mochly-Rosen, PhD, professor of chemical and systems biology and the George D. Smith Professor in Translational Medicine. “A single pharmaceutical agent may be enough to slow progression of several different neurodegenerative conditions.” She is poised to partner with biomedical companies that can help move this agent, known as P110, into clinical trials.
The new strategy came to light through experiments conducted by Mochly-Rosen, postdoctoral scholar Amit Joshi, PhD, and colleagues that implicate two types of normally protective brain cells called glial cells in triggering neuronal destruction. Collectively, these glial cells outnumber neurons in the brain.
Microglia monitor the brain for potential problems — say, signs of tissue injury or invading pathogens — and scavenge protein aggregates and debris left behind by dying cells.
Astrocytes release growth factors, provide essential metabolites and determine the number and placement of the connections neurons make with one another. The experiments, published in October 2019 in Nature Neuroscience, showed that mitochondria can convey deleterious inflammatory signals from microglial cells to astrocytes, and then from astrocytes to neurons.
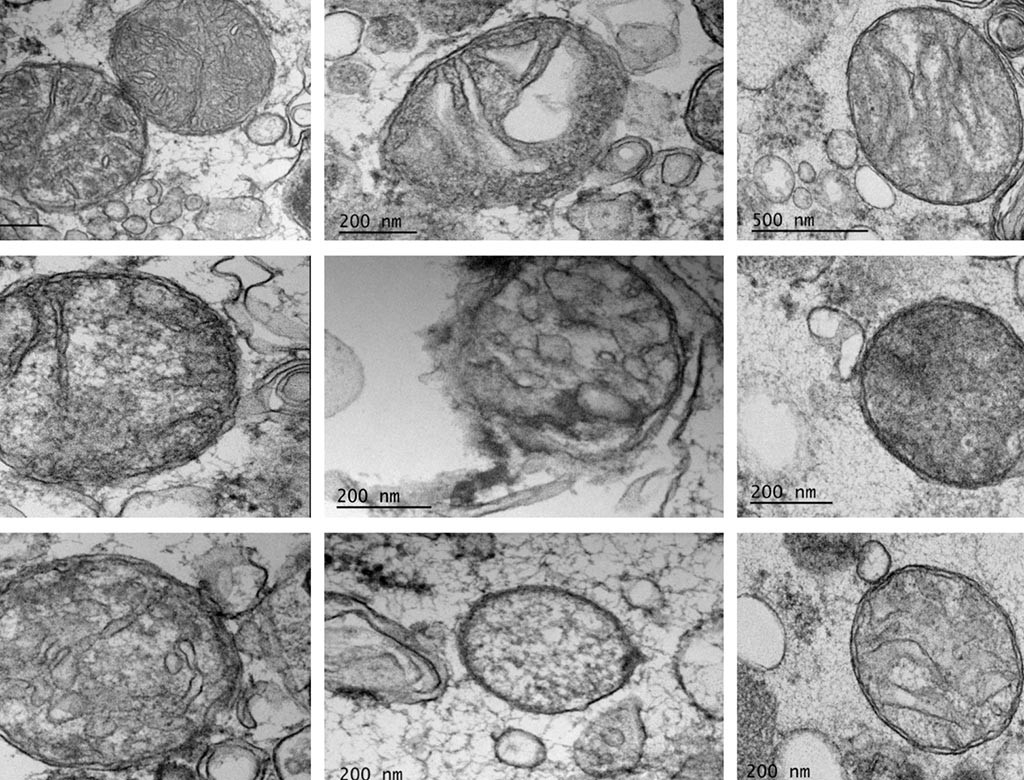
Viewed close up, mitochondria are convoluted tubular networks that are perpetually being right-sized in a dance of fusion and fission. As mitochondria frequently get shuffled from one part of a cell to another, they must shift their shapes to accommodate their environments: Too much fusion, and they become too tubby to get around on the intracellular-transit grid or to work well. Too much fission, and they break into dysfunctional bits.
An enzyme that facilitates mitochondrial fission can be catapulted into hyperactivity by neurotoxic protein aggregates such as those linked to Alzheimer’s, Parkinson’s or Huntington’s diseases, or ALS. About seven years ago, Mochly-Rosen’s team designed P110, a tiny protein snippet, or peptide, that blocks mitochondrial fission when it’s proceeding at an excessive pace, as happens when a cell is damaged.
In the new series of experiments, the researchers kicked microglia grown in culture dishes into an inflamed state by simulating multiple neurodegenerative disorders, in each case by introducing a toxic protein whose aggregation heralds a specific disorder’s onset. The inflamed microglia released some enigmatic something into their culture broth that was able to trigger inflammation in astrocytes that were immersed later in the same broth.
Likewise, a similarly mysterious something released by inflamed astrocytes into their culture broth was able to kill neurons steeped in that broth later.
Mochly-Rosen and her colleagues proved that the inflammatory agent being expelled by both microglia and astrocytes was one and the same: damaged mitochondria. What’s more, adding P110 to the microglial culture dishes substantially blocked this faulty-mitochondria-driven transfer of inflammation from one cell type to the next.
Even healthy cells routinely release mitochondria into their surrounding environment. This can be beneficial if those mitochondria are healthy and can still generate energy.
However, Mochly-Rosen and her co-researchers found that when microglia and astrocytes became inflamed, the mitochondria they released were more apt to be fragmented products of disruptive fission, which are lethal to nearby neurons. And blocking excessive mitochondrial fragmentation with P110 was enough to significantly reduce neuronal death.
“The ratio of damaged to functional mitochondria in the surrounding milieu determines whether neurons survive or die,” Mochly-Rosen said.
The discovery has given her lab a new outlook, she noted: “We humans are as good as these little bacteria inside us. They are the ones who decide our fate.”

