Spring forward
In pursuit of a medical device for children with short gut syndrome

When Lydia Garcia was a month old, she suddenly couldn’t breastfeed. “She kept throwing up, and a lot of my milk was coming out through her nose,” said Lydia’s mother, Noemi Garcia. “Then everything just started coming out green.”
Garcia and her husband, Ellis, rushed their infant to a hospital near their home in Santa Maria, a small town on California’s central coast. Soon Lydia was helicoptered to Lucile Packard Children’s Hospital Stanford, where doctors explained that she had signs of an intestinal blockage.
“We did surgery to find out what had happened,” said James Dunn, MD, PhD, a professor of surgery and division chief of pediatric surgery at Stanford Medicine. “Her intestine had twisted around itself so that a good portion of it had died.”
Over a few weeks in November 2023, Lydia underwent a series of procedures to remove several segments of dead tissue, ultimately leaving her with just 9 inches, or 23 centimeters, of small intestine, about 10% of the normal amount for a newborn.
“We had all sorts of different doctors talk to us about having a baby with short gut syndrome,” Noemi Garcia said. “I had no idea what that was.” She learned that Lydia was in a risky spot: In short gut syndrome, patients have so little intestine that they can’t absorb enough nutrients to sustain themselves. They can’t eat normally, depend on intravenous nutrition and often have a poor quality of life.
At the time Lydia ended up in his operating room, Dunn was in a challenging spot of his own. He had been trying for more than 20 years to develop a medical device that stimulates regrowth of lost intestine — just what patients like Lydia need. But progress on transforming it from a lab-validated concept to a commercially available device approved for infants was slow.
“It takes just a huge amount of effort to take a relatively straightforward device to the patient’s bedside,” Dunn said. This is especially true for medical devices intended for children. Each year, the U.S. Food and Drug Administration approves dozens of new devices for adults, versus just a handful for kids. As a result, some aspects of pediatric medicine lag years or decades behind care for adults.
Why it matters
- The medical device boom has not reached children.
- Stanford Medicine programs are accelerating pediatric medical device development.
- A springlike device is being tested as a way to treat children whose intestines are too short to absorb sufficient nutrients. It works by gently stretching the tissue, which encourages it to regenerate.
The gap is largest for patients with congenital conditions such as heart defects and for diagnoses like short gut that disproportionately affect babies and small children. Several Stanford University experts have formed collaborations with the FDA, with other academic institutions and with people inside Silicon Valley’s innovation ecosystem to address the dearth of pediatric medical devices.
“Babies and children deserve the best, most advanced care we can provide, including medical devices tailored to their specific needs,” said Paul King, CEO of Stanford Medicine Children’s Health. “We want to develop new medical solutions for kids because it opens the door for decades of healthier life.”
When he met Lydia and her family, Dunn didn’t know if he’d be able to offer the new device to his tiny patient. But he had hopes for Lydia and, in his way, which is plainspoken and kind, he was able to transmit that hope to the Garcias during the harrowing weeks when Lydia was undergoing surgeries to remove dead intestine tissue.
“I remember Dr. Dunn coming in the room and reassuring us that she was going to be OK, she was going to get through this,” Noemi Garcia said.
Mind the gap?
In the past 20 years, as medical device innovation for adults has accelerated, the boom hasn’t reached children. Many new supposedly pediatric devices are first developed for adults, then approved only for adolescents, not smaller patients — an inadequate trickle-down approach.
“If you look at approval of devices specifically for children — for their unique diseases and problems — it’s between zero and five per year,” said James Wall, MD, a clinical professor of surgery.
The result, said Janene Fuerch, MD, a clinical associate professor of pediatrics, is that care for babies and small children often relies on jury-rigged solutions.
“We use lots of tape,” said Fuerch, a neonatologist.
She means this literally: Neonatal nurses learn to handcraft three-dimensional supports from medical tape for catheters and other pieces of equipment. In adult medicine, a sterile, prefab device would be used instead.
“We’re treating the most vulnerable population — my patients can’t talk or advocate for themselves and sometimes weigh about a pound,” Fuerch said. “We’re not giving them the most up-to-date and precise medicine, which I find completely unacceptable.”
Wall’s specialty, surgery, is also full of instances in which pediatric experts must improvise. Concern about this inequity has motivated him and Fuerch to lead Stanford’s efforts to accelerate medical device development for children.
The reason so few pediatric medical devices make it from idea to viable product lies in a combination of financial, practical and ethical challenges, the experts said.
“One argument from the medical device industry is that pediatrics involves small markets, and it’s hard to rationalize an investment,” Wall said. Although children constitute 25% of the population — “and 100% of the future,” as Wall likes to say — most kids are pretty healthy.
Insurance reimbursement is another obstacle. To introduce devices for adults, inventors negotiate primarily with Medicare, which insures people 65 and older through a single federal infrastructure. By contrast, Medicaid, which insures about half of U.S. children, is administered by states or counties.
“There are 280 different entities that you need to negotiate with to get reimbursement through Medicaid,” Fuerch said. “It’s really hard for anybody to be incentivized to do this.”
Kids’ anatomy and physiology also change dramatically as they grow, presenting design challenges. A one-size-fits-all adult device may require multiple iterations for pediatrics.
In addition, ethical concerns result in inventors in pediatrics facing higher risk-tolerance barriers from regulators. Small kids can’t advocate for themselves, and regulators worry that new devices might cause worsening or lasting problems for children. So, the FDA often requires safety tests in adults before starting trials in children, although this, too, can raise ethical questions, Wall noted.
“It’s with good intentions that the FDA says, ‘Hey, test this in an adult first,’ but it misses the point that you really should test in the population that can benefit, not on random other people,” Wall said. Caution is appropriate, he added, “but these children have real problems that need to be solved.”
The potential benefits of getting a new device through the approval process are enormous. Effective pediatric medical devices reduce the suffering of kids and their families, cut costs for them and the health care system and, most important, enable children to grow up in better health.
“If you move a child along the arc from disease to health when they’re a year old and they get another 80 years of quality life, it’s really meaningful,” Wall said. “And it probably drives a lot of value for society.
“But who pays for that? It’s unclear who is responsible for paying for that lifetime value of a solution in childhood.”
Stretching what’s possible
Dunn became fascinated with the digestive tract’s ability to remodel itself 25 years ago, when he was a pediatric surgeon-in-training. For instance, he learned that in intestinal atresia — a congenital defect in which an infant is born with two disconnected segments of intestine, one of which is very small — the small piece quickly expands to normal dimensions after the segments are surgically linked.
“I thought it was super intriguing,” Dunn said. “I wanted to learn more about how the intestine does that.”
Around the same time, he also met his first patients with short gut syndrome, babies like Lydia who had lost most of their intestines to volvulus (in which the gut twists on itself, cutting off blood supply), or to a prematurity complication called necrotizing enterocolitis.
Newborns usually have about 6 1/2 feet, or 200 centimeters of intestine. Losing more than half creates lasting problems.
“If they’re down to 40 centimeters, we can count on them being on intravenous nutrition for years, and if they’re at less than 20 centimeters, it may be lifelong,” Dunn said.

Though intravenous nutrition has improved in recent decades — older formulations caused liver failure — it costs more than $200,000 a year and decreases the quality of life for patients and their families. Some children gain enough intestine as they grow to be weaned off IV nutrition, but after months or years of not eating, they are averse to eating by mouth. Intestinal transplants often fail.
The gut is one of the body’s barriers to the outside world, making it difficult to give a just-right dose of immunosuppressive drugs: “It’s a very tight rope to walk between infections and rejection,” Dunn said.
What short gut patients really needed, he thought, was more of their own intestine.
His early inspiration hit when he was listening to a lecture about bones. The lecturer explained the procedure for lengthening a bone in someone whose legs are different lengths: You saw the short bone in half crosswise, brace the sawn ends a few millimeters apart, and let new bone cells fill the gap. A few days later, you enlarge the gap by a few more millimeters and repeat the process until the bone is long enough.
Or, as Dunn describes it, “You break the bone and pull on the bone, and it grows.”
The idea of pulling on a living tissue lodged in his head.
“It struck me, ‘Hey, maybe we can do the same to the intestine. If we stretch it, that mechanical signal will stimulate growth, and you’ll have more intestine as a result,’” Dunn said.
From lab to life
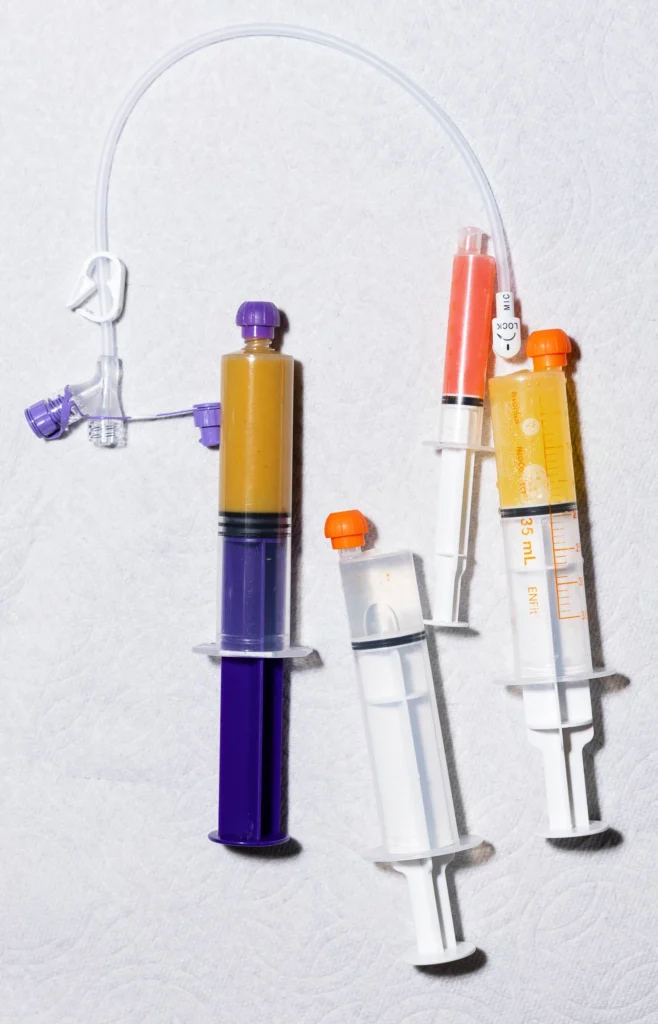
After finishing his training in 2001, Dunn was hired as a surgeon-scientist at the University of California, Los Angeles. For the next several years, his research team tested ideas for treating short gut, eventually designing a spring device that can be sutured inside the intestine to put tension lengthwise along the intestinal wall.

Studies in animals showed that each spring could lengthen the intestine by up to four centimeters. After three weeks, when the spring had fully expanded and the sutures holding it in place dissolved, the device passed out in the animal’s stool, leaving healthy new intestine. Dunn was granted a U.S. patent for the device in 2015.
But he wasn’t sure how to advance his idea to an approved-for-kids, commercially available therapy. In 2016, he came to Stanford Medicine, attracted, in part, by what he could learn from the university’s expertise at commercializing medical innovations. He then began collaborating with Thomas Krummel, MD, his predecessor as surgeon in chief at Packard Children’s and an experienced medical innovator.
Krummel moved into device development in the early 2010s and soon recognized that, to get their ideas to market, his colleagues had to give up on the idea of being, as he put it, “the Swiss army knife that can do everything.”
“Doctors and scientists don’t need to be good entrepreneurs; they need to identify and surround themselves with others with the skills they don’t have,” said Krummel, who is now an emeritus professor in pediatric surgery. He introduced Dunn to a biomedical engineer named Andre Bessette, who became the CEO of the medical device company that he, Dunn and Krummel co-founded, which they named Eclipse Regenesis.
Krummel and Bessette began securing funding for the startup. Dunn had funded his discoveries using grants from the National Institutes of Health, academic societies, patient advocacy organizations and smaller granting mechanisms available to researchers at UCLA. But these pathways wouldn’t cover the cost of commercializing their device. Instead, the team used funding from angel investors and from a seed grant from the UCSF-Stanford Pediatric Device Consortium, which receives funds from the FDA.
They also conferred with private health insurance companies about reimbursement to demonstrate to potential investors that the team’s concept for short gut patients was on solid financial footing.
“The status quo of how we care for these kids is so phenomenally expensive,” Bessette said. Unlike some pediatric medical devices, which might save money for the health care system — but only in the long run — the spring device could quickly benefit patients and decrease costs for insurers by getting patients off of intravenous nutrition, the team told the insurance companies.
“Our device is a much less expensive path to a permanent solution,” Dunn said.
Bessette began seeking FDA permission for a human clinical trial. The FDA requested animal data on device effectiveness from an independent lab, as well as evidence that the company could reliably and safely make the spring device, following good manufacturing practices and using materials that are certified for humans.
“Academics are used to building prototypes in their lab — hand building one-offs — and putting them in animals to look at results. That shows proof of concept, but it’s not a clinical device,” Bessette said. “It’s a big eye-opener for them to see what an actual medical device manufacturing process looks like.”
FDA permission for a human trial came in late 2022, but it had a catch: The FDA wanted the developers to start by testing the device in adults. Short gut syndrome can occur at any age, such as in people who suffer a traumatic intestinal injury.
A 36-year-old man was the first to receive the device in a surgery performed at Stanford Medicine in early 2023.
Widening the device pipeline
Wall and Fuerch are leading several efforts at Stanford Medicine to widen the pipeline of pediatric medical device development. The Stanford Mussallem Center for Biodesign offers a variety of fellowships for trainees and faculty, including in pediatrics, to help them understand the nuances of the medical design process and build networks of experts with the knowledge to help with commercialization. (Wall and Fuerch are both alumni of the program’s innovation fellowships and help teach the current fellows.)
Wall founded a pediatric device initiative at Stanford Medicine in 2014, which expanded into Stanford’s half of the UCSF-Stanford Pediatric Device Consortium, thanks to a 2018 grant from the FDA that made it one of five such consortia around the country. Fuerch now leads Stanford’s part of the consortium; participants meet in weekly think tanks and can enter an annual seed funding competition. Eclipse Regenesis received the top prize in 2020.
In 2022, Wall and Fuerch founded Impact1, a pediatric, maternal and fetal device development program within the Mussallem Center. Co-directed by Fuerch and Kunj Sheth, MD, an adjunct professor of urology, Impact1 helps experts from around the world identify medical problems that a new device could solve through an iterative process of brainstorming and designing potential solutions.
The group also assists inventors like Dunn who have a well-tested idea they hope to commercialize. In the past five years, Impact1 has supported more than 250 projects in 19 countries. (One of their success stories is a device that secures catheters threaded into a baby’s umbilical cord in the neonatal intensive care unit — a sterile, prefab solution that lowers infection risk for a problem previously addressed with lots of tape.)
“We are all entrepreneurs and innovators ourselves,” Fuerch said, of the programs’ leaders. “We’ve all started pediatric health tech companies, and many of us have had technology commercialized and acquired.”
The experience has helped Fuerch and Wall build a network of professionals they can introduce to up-and-coming innovators, including experts in biomedical engineering, regulatory processes, insurance reimbursement, intellectual property, business planning, hospital administration, venture capital and philanthropy.
Understanding that they need this network often requires a mental culture shift for academics.
“I sometimes say to them, ‘You can own 100% of nothing or a part of something. Which do you want?’” Fuerch said. “That’s the really difficult thing — letting go and realizing that there’s a whole other side to this, the execution, which is just as hard, if not harder sometimes, than the idea itself.”
Lydia’s springs
By Lydia’s first birthday, in October 2024, she’d been home from the hospital for a few months and was stable on intravenous nutrition. Dunn and his team had already published a peer-reviewed study of the spring device in the Journal of Pediatric Surgery, demonstrating its long-term safety when used in an animal model.
Following the FDA’s guidance, the team implanted the devices in three adults with short gut syndrome who already needed intestinal surgery. For these patients, the device was safe, and one patient grew enough new intestine to stop using intravenous nutrition. The team published these results in November 2025 in Surgery, the first study documenting how the device works in people.
At the same time, the team kept asking the FDA to let them move the device into children. In mid-2024, they received permission through the agency’s compassionate use pathway to try the device on their first pediatric patient, a preschooler. The pathway allows for case-by-case use of not-yet-approved devices for patients with unusual needs.
A few months later, the same permission was given for Lydia. She received her first spring shortly after her first birthday, and a second in March 2025, becoming the first person to have two springs placed.
She gained a total of about four centimeters of intestine, but that wasn’t the only result that mattered.
Both springs were placed in Lydia’s terminal ileum, the last part of the small intestine, which has special absorptive properties but was mostly destroyed when her intestine originally lost its blood supply. “People who have ileum can come off intravenous nutrition much more readily than those who do not,” Dunn said.
In August 2025, Lydia had a third surgery to reconnect her intestines.
By then, she had spent a significant part of her life in the hospital — she stayed for eight months after the original series of intestinal surgeries — and was not very mobile or gregarious. But after the reconnection surgery, all signs pointed to Lydia feeling better.
“She was a totally different baby. She was climbing up the crib in the hospital,” Noemi Garcia said.
“We saw a big difference in her wanting to crawl,” her husband said.
Lydia now receives intravenous nutrition and nutrients through a gastrostomy tube to her stomach. (The tube allows nutrients to enter her digestive system gradually, helping her absorb more of them.) And, with help from occupational therapists, her parents are introducing Lydia to solid food.
“She’s able to take food by mouth, but not a lot,” Ellis Garcia said, likening her to “a baby bird.” Lydia tends to gag, but the family knows it will take time for her to gain all the skills of eating. “We’ll give her a little portion, and if she doesn’t want it, there’s no pressure.”
The Garcias are grateful that Dunn’s decades of research paid off at just the right time for their daughter. Although her journey hasn’t been easy, Lydia is now a cheerful, chubby-cheeked 2-year-old who is learning to walk and loves to sing — Jingle Bells is her recent favorite.
“It made us happier,” Garcia said of the real-world value of medical research to his family.
“It definitely changed us,” his wife added. “It gave us hope of her being a regular baby, a normal toddler.” The Garcias envision a life where Lydia will enjoy many of the same things as her two older siblings: “She’ll probably be able to play sports and do all of that.”
Eclipse Regenesis has secured FDA permission for a large clinical trial of the spring device in patients as young as 3 months old. It began in September and is accepting participants in five locations.
The FDA will use data from the trial to decide whether to grant final approval to the spring device. Word about the trial has started to spread in the neonatal intensive care unit. Fuerch said she has heard her patients’ parents say, “Oh, yeah, and then he’ll get the coils,” as if this were the most logical thing in the world.
“I always am shocked because it is just so novel,” she said. “This is one of the very few places in the entire world where you could have a chance to get off intravenous nutrition and live a more normal life.”
“As doctors and surgeons, we take care of one patient at a time but if this spring works, we may be helping thousands of patients every year,” Krummel said.
“By developing a new technology that is applied not just in your own hands but also across the world, you maximize the good you can accomplish.”
Although they don’t know how things will turn out for Lydia, the innovators feel growing optimism for her and for all short gut patients.
“My hope is that she’ll be able to come off intravenous nutrition,” Dunn said. “More time will tell. If she doesn’t, she’s still a candidate for additional springs in the future.”
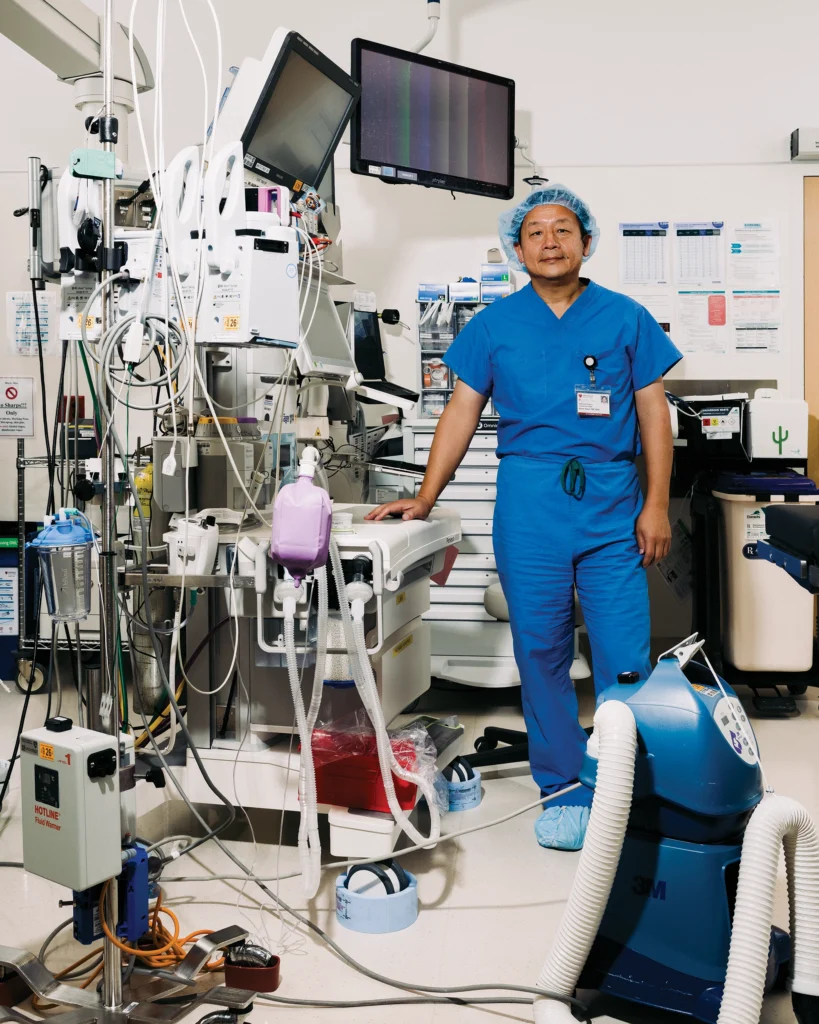
Spotlight on James Dunn
Professor of surgery
James Dunn is a pediatric surgeon and a bioengineer who conducts procedures ranging from the head to the toes — with babies who have birth defects as his most frequent patients. In his laboratory he seeks better solutions for children with short gut syndrome, which prevents them from absorbing enough water, nutrients and electrolytes from food and drink.
- Grew up in Taiwan.
- Was inspired to become both an engineer and a surgeon by his childhood experience of seeing his grandfather walk into the room on two legs after an amputation for diabetes. This walk was made possible by a prosthetic device.
- Relaxes by playing beach volleyball most Fridays.
- Strategy for overcoming challenges: “Think about something different. Solutions and ideas will come to you.”
- The medical device Dunn developed to lengthen the intestines was inspired by his desire to understand how our tissues adjust to different situations. “The body is just amazing,” he said. “It can adapt in ways that are super fascinating.”
In his words: “The best part of my job is seeing kids get better.”

