India’s medical miracle
The world’s largest ambulance system

Hyderabad, India — One sultry evening in late July, Suresh Bojja entered the swirling vortex of traffic in this burgeoning south Indian metropolis. The roads here are a microcosm of life in India, as man and vehicle feverishly compete for every inch of space in a desperate effort to move forward, or even just survive.
Bojja had just finished his shift as a transit supervisor for Amazon and climbed on his motorbike to navigate through the cars, trucks, buses, rickshaws, motorbikes, bicycles and pedestrians that choke the streets, the air filled with exhaust and the relentless cry of beeping horns.
Suddenly, three people on a single motorcycle headed directly into his path, sending him flying into the air and onto the ground. In a fit of road rage, fueled by alcohol, the trio then pummeled him in the head, face and stomach, leaving him for dead on the pavement.
In the not-too-distant past, Bojja likely would have met his end there, as medical aid was virtually nonexistent on India’s roadways, the site of 10 percent of the world’s traffic deaths.
But today India has created what some once considered unimaginable: the world’s largest ambulance service and the first of its kind in the developing world, which reports saving more than 1.4 million lives in its first 10 years. The system, known as GVK EMRI (Emergency Management and Research Institute), is a centralized 911-type network in which members of the public can call a single number to summon a team of trained professionals to provide aid en route to the hospital for a wide range of medical emergencies.
Online extra:
In minutes, an ambulance crew rescued Bojja and brought him to Gandhi Hospital, the nearest government facility, where he lay in a coma for 2 1/2 days. Two weeks later, he stands in his brother’s tidy two-room apartment, his left eye visibly damaged enough to frighten away his two children. But he is upright and his mind clear as he quietly thanks those who came to his aid.
“The ambulance reached me in time,” he says in halting English. “If not, I might have lost my life from my injuries. My life is a present — they saved my life. I am very thanks for that.”

On Aug. 15 — India’s Independence Day — hundreds of GVK EMRI officials as well as 10 faculty and staff members from the Stanford University School of Medicine celebrated the 10th anniversary of the system at its headquarters, festooned for the occasion in orange, yellow and green marigolds. Begun with just 14 ambulances in one state, GVK EMRI has expanded to a fleet of nearly 10,000 ambulances, manned by some 20,000 medical professionals who ply the roads in cities and rural villages to provide access to emergency care to 750 million people — three-quarters of India’s population. It continues to expand, with G.V.K. Reddy, EMRI’s chair and managing director, announcing at the celebration that he had just inked an agreement with Sri Lanka to bring the service there, likely by the end of the year.
The public-private nonprofit provides its services free of charge, and 85 to 90 percent of its beneficiaries are the poorest of the poor.

“It’s amazing to see what’s been accomplished in a very short period of time. It’s very inspirational to me,” Lloyd Minor, MD, dean of the School of Medicine, told the crowd at the festivities. “Today’s celebrations are an opportunity to affirm our collective commitment. We look forward to working with the leadership on more programs in the future.”
Stanford Medicine physicians have been instrumental in helping bring the system to life, training the country’s corps of paramedics and designing India’s first emergency protocols — a 108-page tome of emergency care that is carried on every ambulance. Stanford physician-scientists also conduct research on emergency trends that continuously guides improvements in patient care.
“It’s hard to fathom what this system has done in 10 years,” says S.V. Mahadevan, MD, interim chair of Stanford’s Department of Emergency Medicine and founder of Stanford Emergency Medicine International, which brings emergency medicine programs to countries as far-flung as Mongolia, Cambodia and Myanmar, and provides medical expertise to GVK EMRI. “It could be regarded as one of the most important advances in global medicine in the world today.”
A grand vision

In the spring of 2005, Mahadevan received an unexpected visit in his Palo Alto, California, office from an Indian businessman, Venkat Changavalli, who had flown halfway around the globe for the sole purpose of meeting with him. Changavalli described a grand plan to set up a countrywide ambulance system in India and broached the idea of a partnership with Stanford. Mahadevan was deeply skeptical, as something like this had never been accomplished before in a developing country, particularly one as large, diverse and bureaucratic as India. After the meeting, he drove Changavalli to San Francisco International Airport without signing on, assuming he’d never see him again.
“I remember thinking, ‘This guy wants to start an ambulance service that covers all of India. It will never happen,’” recalls Mahadevan, an associate professor of emergency medicine. To his great surprise, he received an invitation a week later to the launch of the new service on Aug. 15, 2005 — a service they hoped to improve and expand with Stanford’s expertise. He decided to travel to India for the ceremonies and came away impressed with how the founders had adapted India’s legendary call-center technology for use in the medical arena, he says.
‘I remember thinking, “This guy wants to start an ambulance service that covers all of India. It will never happen.”’
The system was launched by a passionate group of business and medical professionals who wanted to rescue the countless people dying from treatable injuries and illness simply because they had no way to get to a hospital in time, Ramana Rao, MD, DPH, director of EMRI’s emergency medicine learning center and research, says in an interview in his office.
“Most of the time they were waiting for the graces of God,” Rao says. “Some people made attempts by rickshaws, bullock cars, taxis, three-wheelers and sometimes bicycles. People would put a cot on their shoulders and carry someone down from the top of the hill. Out of desperation, they were using every mode of transportation.
“Poor people are dying for simple reasons,” he says. “My heart throbs for that.”
Rao, who has been with EMRI since the start, is a bespectacled man with jet-black hair, a warm smile and an earnest demeanor, often leaning forward in his chair to reinforce his points. He is essentially EMRI’s chief medical officer, constantly looking for ways to improve patient care.


Rao says the system became possible because of two critical developments in India: the construction of a comprehensive road system and the communications revolution that has put 950 million cell phones into people’s hands, including those of the rural poor. “People may not have a square meal, but they have a mobile phone,” he says. “So it was a synergy of many technologies.”
The number 108 was chosen for the toll-free service because it is considered an auspicious number in multiple religions prevalent in India. The service was launched on a small scale in Hyderabad, a sprawling mega-city of about 7 million people, in which gleaming malls and office buildings housing high-tech companies such as Google, Oracle and Cisco mingle with 16th-century Moghul monuments and the grit and decay of poor neighborhoods. The central call center there now serves the 83 million people in the states of Andhra Pradesh and Telangana.
EMRI has replicated the network in 15 states across a broad swath of this country of 1.2 billion, the second most populous in the world. It deploys five boat ambulances in the tea-producing state of Assam, in the country’s northeast region, where the Brahmaputra, one of Asia’s major rivers, snakes through the province. And there are ambulance rescues in the farthest reaches of the Himalayas, made possible by the construction of roads to access patients.
Each state contributes to the system, as does the federal government. Together they provided a total of $156 million in financing in 2014 — the equivalent of 1 rupee (about 2 cents) per citizen per month, says Krishnam Raju, EMRI’s director. The system also depends on private philanthropy, with initial support provided by Ramalinga Raju, former chair of Satyam Computer Sciences. When he ran into financial trouble in 2009, the organizers turned to industrialist G.V.K. Reddy, who agreed to rescue the system, contributing $250 million to date through his family foundation. Reddy, 78, is a self-made billionaire, the son of a farmer, who has not forgotten his roots.

“I strongly believe in giving back to society by reaching out to the masses,” he says. “It couldn’t have been fulfilled better than providing emergency care and saving lives. It gives me immense satisfaction that EMRI 108 services … are reaching out to the poorest of the poor in rural areas.”
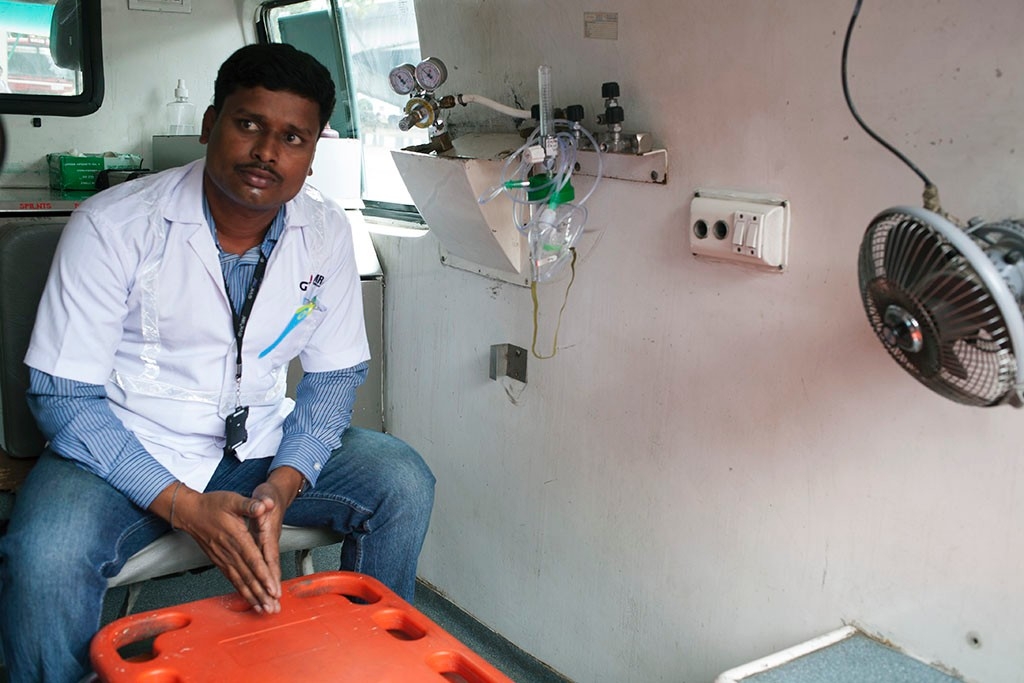
The funds are used to pay salaries and buy ambulances, designed and built in India to accommodate local needs. The vehicles are constructed differently from ambulances in the United States, as they include a side bench to carry as many as five or six family members along with the patient.
Though the government was able to supply needed equipment from the outset, India had no paramedics or emergency medical technicians to staff the vehicles, so officials began searching for a partner to help train an entirely new class of medical professional. That’s how Changavalli ended up in Mahadevan’s office.
“We were looking for who is best in emergency medicine and we did a Google search and found Stanford. And there, we found Dr. Mahadevan, which means great God in Hindi,” Rao says with a smile.
Mahadevan is a native of Oakland, California, but his parents emigrated from India, a connection EMRI officials hoped would endear the project to him. He began working as a consultant for the group in 2005, and by 2007 the School of Medicine had signed a formal agreement to develop an educational curriculum and train an initial group of 150 highly skilled paramedics and 30 paramedic instructors.
‘We were looking for who is best in emergency medicine and we did a Google search and found Stanford. And there, we found Dr. Mahadevan, which means great God in Hindi.’
“The goal was to have them replace us as instructors,” Mahadevan tells Stanford students in a class on global entrepreneurship. He is a tall, lanky man with a gregarious nature who has won numerous awards for his teaching and his clinical expertise. In the early days of the project, he spent nearly as much time in India as he did in California, focused on training the new caregiver-educators.
“We saw an amazing transformation. These novice teachers became experts,” he says. “They devoured our teaching approach. … The day our first group graduated in 2009 was one of the proudest days of my life.”
“The contribution from Stanford is something very phenomenal,” Rao says. “Back in 2007, there were no programs to train advanced paramedics. I’m proud to say that Stanford physicians have trained advanced clinical educators who have maintained our standards. Down the line, these educators will become the leaders in our country.”
The Indian government also invested in educating a cadre of emergency medical technicians, who receive less training than paramedics but have the skills to manage the daily influx of medical emergencies. When an assessment found them lacking in certain subjects, Stanford physicians stepped in to supplement the EMT curriculum with refresher courses to improve their performance.
Peter D’Souza, MD, clinical assistant professor of emergency medicine, was one of the Stanford faculty who volunteered as a trainer, in part because of a personal experience, he says. He had seen the impact of the emergency-care gap firsthand when a cousin in the south Indian metropolis of Bangalore suffered an injury to her spine in a traffic accident in the 1990s. “People picked her up and put her in the back of a rickshaw,” recalls D’Souza, whose parents are from India. “She had a broken spine and ended up paralyzed. My mother always said, ‘Had she been treated properly, she might be able to walk today.’”
Preparing paramedics
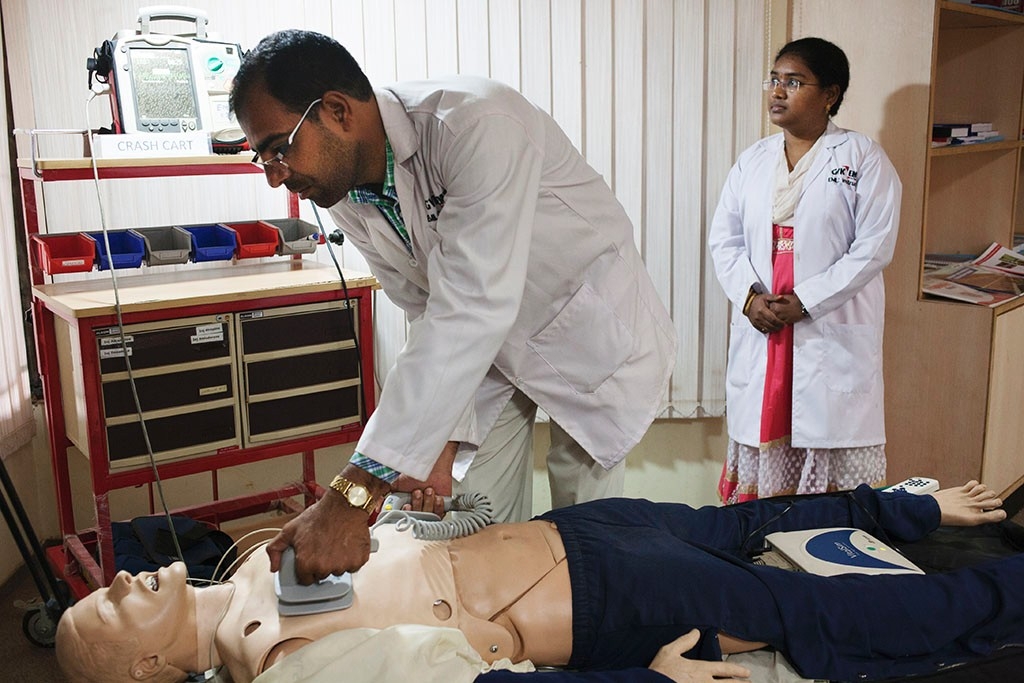
In a classroom at EMRI headquarters, on the northern outskirts of Hyderabad, paramedic instructor Rafi Baigmirza is pounding on the chest of a patient in ventricular fibrillation, a dangerously abnormal heart rhythm. The “patient” in this case is a sophisticated manikin that coughs, screams and breathes to emulate real-life medical situations.
“It’s a chance to treat someone critically ill and make mistakes and learn from your mistakes so you can correct the situation in real life,” Mahadevan says of the simulation training.
In a neighboring classroom, Matt Strehlow, MD, clinical associate professor of emergency medicine at Stanford, is delivering a lecture on the basics of heart disease — the No. 1 killer in India — to 60 men and women, all second-semester paramedic students enrolled in the two-year training course. The students are often shy and tentative at first and have to be coached in how to establish a presence in chaotic situations, particularly roadside accidents, which tend to attract boisterous and unruly mobs of people who can interfere with treatment.
When the early crop of paramedics first began working in the field, they were an unknown quantity and often faced hostile crowds.
“You need to speak with your paramedic voice — be friendly and in charge,” Strehlow tells the group.
The chaos is evident on a recent August afternoon, when the EMTs respond to a call involving a 19-year-old college student who, in the course of turning left, was hit in the flank by another motorcyclist. The student was thrown from the bike and landed on the pavement, briefly losing consciousness. The EMTs hoist him into the ambulance, wrapping his injured right wrist in gauze and cutting open his right pant leg to splint a fractured limb. Several dozen onlookers gather, and there is much jostling and pushing as one gawker shoves a reporter aside so he can snap a photo of the action on his tablet computer.
Strehlow says that when the early crop of paramedics first began working in the field, they were an unknown quantity and often faced hostile crowds. He recalls one case in 2007 in Hyderabad in which a neighbor called 108 to report two children who had been tied up and abused.
“We arrive and there’s this huge crowd. The EMT looks at us and tells us to stay in the ambulance,” he says. “People were yelling and rocking the ambulance. They didn’t trust us. They didn’t understand. They were afraid.”
Today, however, the emergency responders are welcomed with open arms. Sometimes they deliver such good care that patients don’t want to leave the ambulance to enter the hospital, where treatment standards are highly variable, he says.
“It’s remarkable how they were able to turn the tide of public thought,” says Strehlow, the new director of Stanford Emergency Medicine International. “They are cheered. People trust the EMTs and that the system is working for them.”
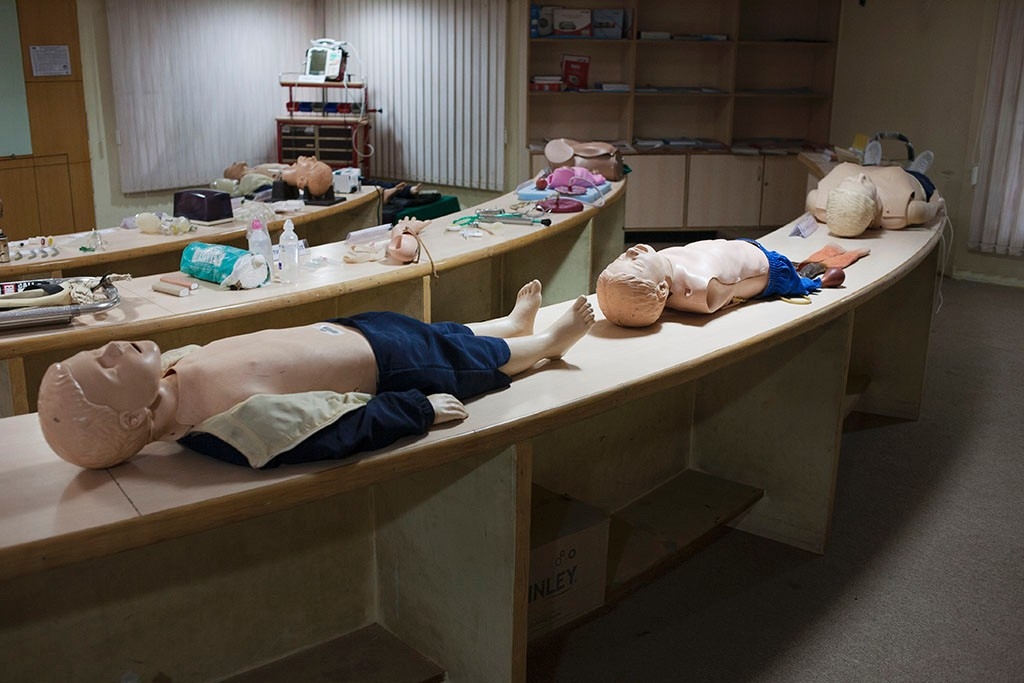

In training the paramedics, the Stanford instructors had to tailor the curriculum to local needs, which are very different from those in the United States. For instance, about one-third of calls to the system, particularly in rural villages, are from pregnant women in labor, who traditionally deliver babies at home, often at great risk. In the past, the maternal mortality rate in India was very high, as women frequently died of complications, such as hemorrhage, infection or obstructed labor. In 1990, for every 100,000 women giving birth, 560 died, according to data from the World Health Organization, the World Bank and the United Nations. The Stanford team has since designed a specialized obstetric curriculum and helped create the country’s first protocols for obstetric care.
“For us, it’s like a bible, a commandment,” Rao says of the protocols. “We are very proud to bring international standards of care to our country with the help of Stanford.”
EMRI also established a separate call number, 102, for free transportation to and from the hospital for women in labor. It now deploys 3,000 ambulances in eight states specifically for this purpose. The maternal mortality rates have dropped significantly — to 190 deaths per 100,000 in 2013 — and Rao says he believes EMRI’s work has played a key role in helping save many women in labor.
The training curriculum also had to take into consideration other common medical problems in India, such as snakebites and pesticide poisonings. Drinking pesticide is a frequent method of suicide in rural villages, especially when the monsoon rains are sparse and crops fail; hopeless farmers see no other way out. Paramedics are now trained to administer atropine, a drug that counters the effect of these toxic chemicals.
Stanford physicians also learned that Indians aren’t prone to some of the medical issues that frequently confront emergency personnel in this country. For instance, peanut allergies, which are common in the United States, are rare in India, D’Souza says. When he presented a lecture on the subject to would-be paramedics, “most of the students didn’t even know what I was talking about.”
One of the plagues of the emergency system, particularly in urban areas, is roadside accidents, which account for 12 percent of calls. The mortality rate among traffic accident victims is immense in India, as few people wear safety helmets or take other precautions, and in the past, many failed to get care in time, Mahadevan says. Moreover, before the 108 system was introduced bystanders were loath to become involved since accidents were the province of the police: They feared they’d be implicated in the injury and hauled off to jail, he says. As a result, victims often remained by the roadside, unattended.
“Now bystanders can call the emergency number and have a role in saving someone’s life,” he says.
The hub
The Hyderabad hub for the emergency system is a call center the size of two basketball courts, filled with a hum of voices and rhythmic tapping on computer keyboards as emergency responders in white coats answer the phone to 108 callers. More than 50 call operators, all fitted with headsets, are arrayed in circles inside blue and yellow cubicles that fill the cavernous space. A dashboard on the wall displays in red, yellow and green the number of calls waiting or active; officials are proud of the system’s record in responding to 96 percent of calls within the first ring.

The operators, who speak English, Hindi and Telugu, the local language, quickly gather essential details and enter these into a template on the computer screen: name, phone, location, chief complaint.
This call center alone responds to between 27,000 and 30,000 calls a day from residents in Andhra Pradesh and Telangana. Only about a quarter are true emergencies. The operators remind callers that the number is not to be used for idle chat; those who make repeated nuisance calls are warned they will be reported to the police if they continue to abuse the system.
It’s a far more sophisticated system than in the United States, where the 911 network is highly decentralized, with calls handled county by county according to variable standards, Mahadevan says. “They are very efficient, compared to us,” he says.
On a Thursday afternoon in August, an operator relays a call via mobile phone to emergency medical technician Banothu Mangilal, who has been waiting with two colleagues in one of the ambulances strategically placed around the city of Hyderabad. Mangilal, 28, who is from a poor family in the countryside, says he was inspired to sign up for EMT training about three years ago after his mother suffered a hip fracture in an accident and got help through the system. The work, he says, is immensely satisfying.
“After a night shift of four or five cases, I can go home and tell my wife or parents how I have saved one person,” he says in Telugu through a translator.

On this day, the call involves an older woman who is unconscious. Because many homes lack specific addresses, Mangilal uses landmarks, such as temples or retail stores, to help locate the patient, who lives in a tumbledown neighborhood of cement-block apartment houses, where painted green balconies and blue awnings mix with a tangle of electrical wires and hanging laundry. He and his colleagues maneuver through a thicket of cars, trucks, motorcycles and rickshaws, arriving at the second-floor unit — a dark, closet-sized room occupied by a single bed — where 72-year-old Lalita Anand lies in a brown dress, eyes closed, unresponsive. Her son, Ranesh Anand, had arrived that morning from Mumbai to discover his mother, a recent cancer patient, in a terrible state, unable to speak. He called 108. A strong odor in the room greets the EMTs, who don facemasks as family members scurry to get the patient ready to go.
A brief exam reveals the likely source of her distress: a baseball-sized bedsore on her back that has become infected and may have led to sepsis, a potentially fatal condition, says Strehlow, who is observing the EMTs today. The EMTs give the patient oxygen and start an intravenous line for fluids, then gently lift her onto a backboard and maneuver her down a narrow stairwell.
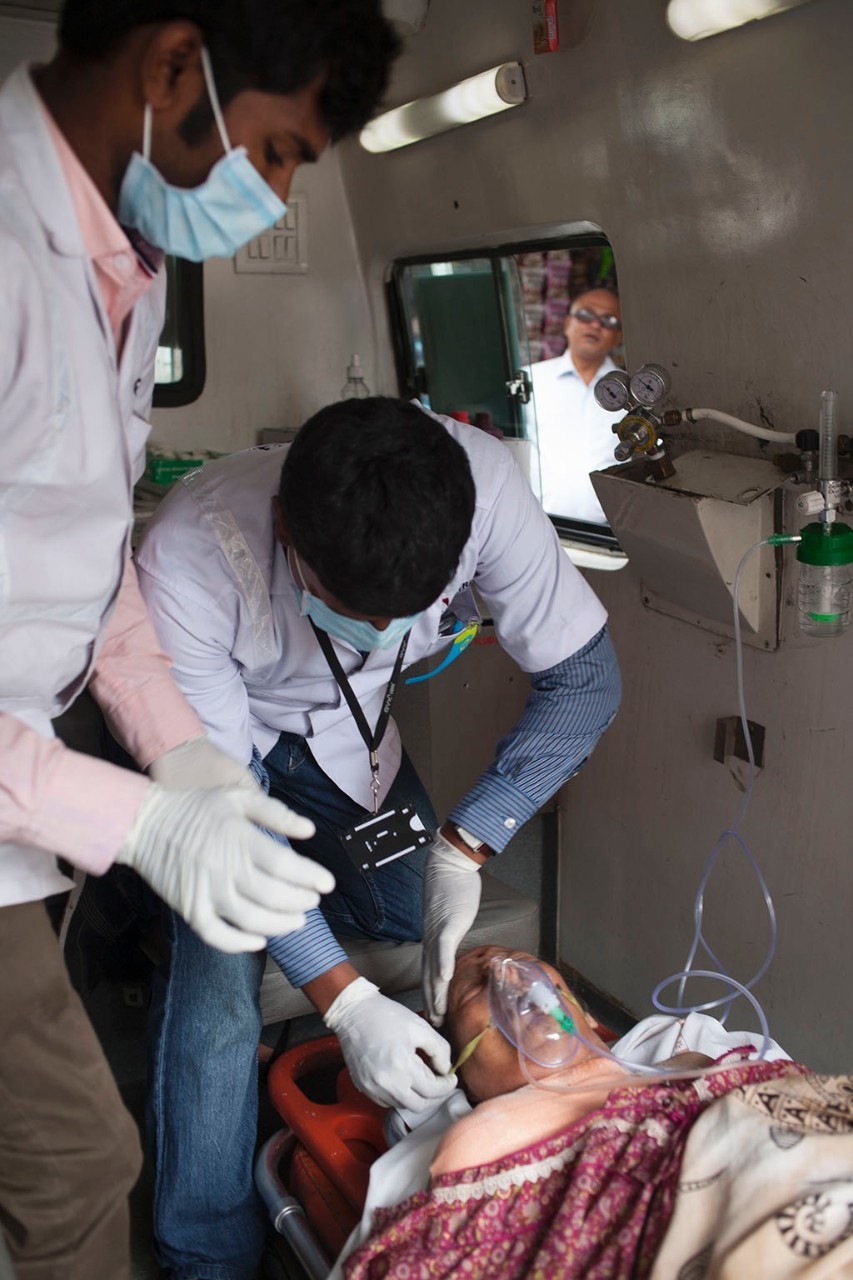
Three family members climb into the ambulance, which arrives at Prime Hospital, a teeming, well-appointed private facility requested by the family. EMRI has signed agreements with many private hospitals that will treat patients free of charge for the first 24 hours. Then the patient may stay there or move to a government facility, where care is free. Many families choose the private option, even though they may have to bankrupt themselves to pay the bills, because they know the care will be better.
In an emergency room bay, Lalita Anand begins to revive. Her eyes open and she responds to questions. Her relatives are beaming.
“Because of GVK, we have care,” the son says. “Everything is normal. … We congratulate them and now we have to pray to God for her to recover. They have provided excellent service. We will remember it for a long time.”
Tracking trends
Because EMRI’s computerized system can capture massive quantities of data, researchers for the first time can track health-care trends and spot problems that need to be addressed. For instance, in one study, scientists from Stanford and EMRI tracked all patients in Andhra Pradesh in July 2009 who called with complaints of chest pain — a total of 585 individuals. They found an “alarming early mortality” rate, with 23.2 percent dead within a month. Many were arriving too late to the hospital to be saved, Mahadevan says. As a result of the study, published in 2010 by the American Academy of Emergency Medicine, most ambulances now carry defibrillators to revive patients in cardiac arrest.
In another study, the scientists looked at more than 1,000 adults and children suffering seizures — the most common neurologic emergency in India — over a two-month period in the state. They found that only 14 percent of these patients were given anti-seizure medications, and 5 percent were dead within a week. The ambulance procedures lacked instructions for patients with seizures, so the Stanford team corrected that with new guidelines and made sure that all ambulances carried anti-seizure medications, typically benzodiazepines.
Currently, the Stanford team is working with EMRI to collect data on burns, which are “horrendously common and often very severe — a pretty big challenge,” Strehlow says. According to the WHO, more than a million people are moderately or severely burned in India every year, compared with 40,000 patients with burns needing hospitalization in the United States in 2008 (the latest figures available).
Indian women typically cook on gas cooktops, and their loose-fitting nylon saris may accidentally brush against the flames, he says. But tragically, many burns are intentionally inflicted by the patient, a partner or another individual, says Jennifer Newberry, MD, JD, an instructor in emergency medicine who is leading the study.
Newberry decided to do the study after seeing some figures from a previous study of burn patients who called the 108 line. Her preliminary analysis of a sample of 434 burn patients who contacted the service over a 90-day period shows nearly half of all burns were intentionally inflicted. Most of those with intentional burns were young married women.

The overall mortality rate for burn patients is high, with 69 percent dying within a month, Newberry’s early analysis shows. By contrast, in the United States, most burn victims survive, even if their burns cover as much as 90 percent of the body, Strehlow says. Among other things, the researchers are looking at survival rates at both public and private hospitals and the levels of care provided.
Improving physician skills
Now that patients are arriving in large numbers at hospital emergency rooms, the hospitals are under pressure to improve the quality of care. But this remains an enormous challenge in a country where the concept of emergency care is very new and fewer than 1,000 emergency physicians practice.
At Gandhi Hospital, a government-run facility in the central city here, an ambulance pulls up to the emergency room door on a Friday afternoon. Medical professionals deliver a patient on a gurney, his blue jeans and T-shirt spattered with red and his right arm in a blood-soaked bandage. The patient, a man in his 20s found injured along the roadside, is still conscious but in severe shock due to blood loss from a gaping wound on his right hand.
EMTs wheel him into the emergency room, where caregivers begin to irrigate the wound, which drips blood over a trash can, and hook him up to an intravenous line. Strehlow, who has been observing the action, says the patient could survive if he gets a transfusion and manages to avoid infection in this hospital, where the walls are peeling plaster, the bed linens are stained and a pile of medical waste and garbage lurks outside the window.
It’s a grim scene where about a dozen patients, many in critical condition, lie on gurneys awaiting care from the only physician in attendance. A man in the corner with a bony chest is heaving in great distress; he desperately needs oxygen, but the staff isn’t there to deliver it.
Despite the chaos, Strehlow says things have marginally improved. About eight years ago, when he visited the same emergency room, he saw two women on gurneys in severe respiratory distress, dangerously close to death, without any aid in sight. In the back room, Strehlow says he found a physician, feet up on the desk. The physician told him, “What do you want me to do? I’m an ophthalmologist. I don’t know what to do,” Strehlow recalls.
At least now some patients are starting to get urgent medical attention as the public clamors for hospitals to respond.
“Now that the concept of emergency care has been introduced, the public is applying external pressure for desperately needed care,” he says.
To help meet the demand, Stanford and EMRI are working to beef up the skills of the generalists who staff emergency rooms, particularly in the government-run district hospitals in rural areas. They have developed a short course for these physicians on how to triage emergencies in both adults and children and how to assess a patient’s condition when expensive tools such as MRI and CT machines are unavailable, Rao says.
Expanding horizons
That is just one of EMRI’s initiatives as it pursues its ambitious agenda. The service aims to double the number of ambulances to 20,000 within the next five years and reduce the average response time in urban areas from 15 minutes to 10 minutes, director Krishnam Raju says. And it plans to extend the service to the entire country and beyond. At the Aug. 15 celebration, chairman Reddy said that in addition to the Sri Lanka expansion, he has approached Indonesia and Thailand to introduce the model there as well.
In India itself, Raju says he believes the 108 service will add at least another five years to the current 67-year life expectancy. And EMRI will continue to work in partnership with Stanford as it expands and brings India into the modern age of emergency care.
“We look forward to another decade of continuing to improve care,” Mahadevan says. “It’s only in its infancy. Over time, I’m confident it’s going to deliver the same level of care available in other countries.”

