All for one
Building a culture of teamwork in emergency care

Early one August morning before the new Stanford Hospital had opened, about 20 nurses, physicians, physician assistants and technicians squeezed into a room at the hospital’s Marc Andresseen & Laura Arrillaga-Andreessen Emergency Department.
It was time for the 7:30 a.m. daily “huddle,” when they learned about the patients they would inherit from the night shift. Thirty had been admitted to the hospital through emergency — “a whopper of a night,” according to Patrice Callagy, RN, executive director of emergency services.
Patients had come in fearing they were suffering heart attacks, complaining of abdominal pain and experiencing headaches — typical emergency cases, just a lot of them.
Because too few beds were available, Karen Stuart, RN, manager of emergency services, asked the team to determine which of the patients could be treated on gurneys outside the patient rooms. Once the new hospital opened, the department’s space would more than double in size, but that was still three months away.
Stuart urged the group to keep track of equipment — a resident had taken an eye-pressure reader to another department — and reminded them to complete their paperwork. Then she asked for “shoutouts,” and a technician praised a coworker who had deftly whisked two patients away from another, who had become agitated.
These huddles, which take place four times a day when employee shifts overlap, ready emergency department workers for the shift ahead. But they also provide opportunities to share information broadly, so members of the team can step outside their roles if necessary. Anyone, regardless of job title, is encouraged to raise a concern, praise a coworker or ask a question.
And every Friday, a faculty member teaches the whole crew a particular aspect of emergency medicine, whether it’s how to communicate with family members, use new equipment, manage blood loss or treat epilepsy.
Typically, physicians aren’t trained to work with people in other health care professions, such as nurses and physical therapists, though all of them care for the same patients.
“Medical training is very siloed,” said Megan Mahoney, MD, vice chief of staff for Stanford Health Care. Most health care organizations don’t reward physicians for working well with others. Stanford Health Care is an exception, Mahoney said.
But as medicine has become more complex and specialized, taking advantage of each team member’s skills is growing in importance. For example, members of a team scheduled to perform a cesarean section learn ahead of time what role each will play so together they can perform the procedure safely and efficiently.
But good teamwork also requires a shift from the traditional, top-down medical culture to a more level playing field. “Nurses need to be able to tell doctors if they see something that concerns them,” said Andra Blomkalns, MD, chair of the emergency department and a champion of empowering every member of the clinical staff. “Anyone should be able to say, ‘I don’t feel comfortable with this.’”
Throughout Stanford Medicine, clinicians are training to promote teamwork. They use standardized exercises and develop their own. Three examples from the emergency department — designing the work space in the new hospital, holding Lego-building competitions and running simulations of treating a pregnant trauma patient — illustrate some of the creative ways Stanford Medicine is building a collaborative culture.

Design with teamwork in mind
About 10 years ago, as physicians and administrators at Stanford Health Care were envisioning the new hospital, they realized that the layout of the new work spaces could help facilitate more collaboration. “With the opening of the new hospital, there was an incredible opportunity to espouse teamwork,” Mahoney said.
Clinical leaders in the emergency department invited various constituents — patients, lab technicians, guest services members, physicians and nurses — to create their ideal department. They placed empty moving boxes around an unused room on campus, marking the ambulance bay, the registration desk, the laboratory and other service locations.
As they acted out typical scenarios of patients arriving with complaints ranging from chest pain to a head cold, they rearranged the boxes until they were satisfied they had the most efficient configuration — one that would ensure a rapid resolution for any condition.
For example, to encourage collaboration and efficiency, the new department has six zones, each featuring a “pod” surrounded by patient rooms. The pod is a group of desks formed into a square, with 10 or so computer screens. The computers belong to everyone, meaning a physician assistant can sit down between a lab technician and a translator, tap her badge on the reader and access her own data.
“… A pharmacist may overhear an attending physician and a resident talking about medicating a patient and can butt in to say the patient is allergic to that medication.”
“It creates a faster pace for treatment, faster decision-making,” said Vasiliy Rodin, RN, assistant care manager, who was in charge of the transition to the new ED.
Everyone can hear others’ conversations, and that’s the idea, Callagy said. “For example, a pharmacist may overhear an attending physician and a resident talking about medicating a patient and can butt in to say the patient is allergic to that medication.
“Or a social worker can overhear two nurses talking about an 80-year-old patient who keeps coming in after falling,” she added. “They can say, ‘That’s someone who needs a referral to the Farewell to Falls program,’ and make that happen.”
The designers of the new department also reworked the entryway: Two teams — each including a registration clerk, a nurse and a medical technician — wait at podiums to greet arriving patients, then get to work immediately. The registration clerk gathers the patients’ information as a medical technician takes their vital signs and the nurse determines the severity of their condition. “It’s like during an auto race, when a car pulls into the pit stop,” Callagy said. “The team works together to get the car quickly back into the race.”

Lego communication exercise
Emilie Wagner, a lecturer at the Hasso Plattner Institute of Design at Stanford, was brainstorming with her husband, Alexei Wagner, MD, an assistant professor of emergency medicine, a couple years ago about a course she was teaching on communication in the operating room.
“We were trying to figure out a way to simulate an operation,” Emilie Wagner said. “We asked ourselves, ‘What can people build together?’ We realized assembling Legos could be a stand-in for the procedure, and we could design an activity that mimics the communication dynamics of a real-world operating room.”
The couple devised a three-person exercise that involves a pile of Lego bricks and a manual with wordless instructions on how to build a model helicopter. One person describes the instructions, similar to how an attending physician instructs an intern; a second, acting as a nurse, selects the pieces; and a third, filling the role of an intern, fits the pieces together.
In the exercise, the person playing the attending physician might tell the one playing the nurse, “Pick out the two dark-blue pieces that have six bumps on them,” then tell the person playing the intern, “Place the pieces on either side of the white square with their shorter sides touching the white square.”
During the exercise, participants wear masks and gloves, as if they were really working on a patient, and they’re hearing pre-recorded background noise from the ED. The teams are also under time pressure as they compete against other teams. “It’s very reminiscent of what it’s like to do a high-risk procedure,” Alexei Wagner said.
“They can have a difficult conversation pretty easily because they’re just talking about Legos.”
Emilie Wagner, a lecturer at the Hasso Plattner Institute of Design at Stanford
The exercise teaches the importance of using precise language and listening attentively, but it’s most effective if participants step into different roles. When he runs the exercise for emergency department personnel, Wagner instructs the real-life attending physicians to act as interns, the interns to play physicians, and the residents to act as nurses.
He wants attending physicians to realize how difficult it is to follow unclear instructions and how someone’s tone of voice can affect outcomes. He hopes interns understand that while they may feel inadequate, their team members often disagree.
“It’s an easy, low-cost, low-risk exercise to learn what it’s like to walk in someone else’s shoes,” he said. “In emergency, when a team is unsuccessful, it’s easy to blame the intern. But maybe the instructions were the problem.”
Wagner oversees Lego exercises on occasion, for new clinicians and others who are interested in trying it. Emilie Wagner said that physicians are willing to participate, and afterward discuss what they learned — including how they failed — because they’re dealing with toys, rather than patients or even manikins.
“They can have a difficult conversation pretty easily because they’re just talking about Legos,” she said.
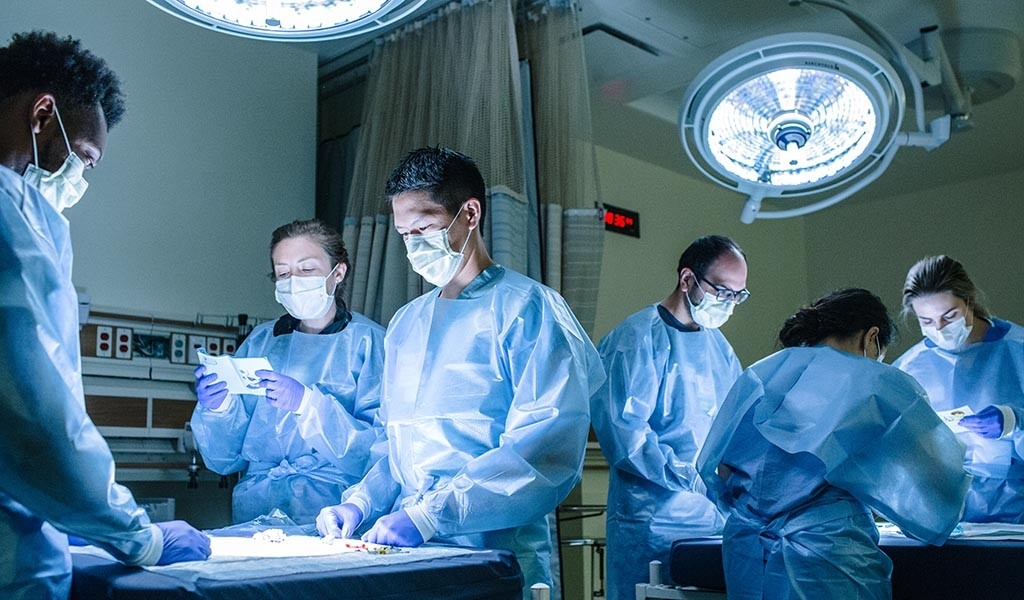
Maternal simulation
In a recent simulated trauma scenario, physicians and nurses crowded around a “patient” lying on a gurney. Kimberly Schertzer, MD, playing the role of a paramedic, announced that the patient had been in a freeway accident, was 32 years old and was 33 weeks pregnant. Everyone acted as if the manikin on the gurney with a distended belly was really a pregnant trauma victim.
The physician in charge stood at the foot of the bed, arms crossed, asking questions about the patient’s vital signs and ordering tests. An emergency physician checked her breathing, her blood pressure and her limbs to see if any bones were broken. An obstetrician listened to the fetal heartbeat.
A nurse sitting behind a screen provided the voice of the patient; her moans echoed through a karaoke machine hidden under the gurney. “My stomach hurts,” she said. “Is my baby OK?”
“The baby’s OK,” an obstetrician answered. The physicians discussed the possibility that the placenta had separated from the uterus, which can happen after trauma, but they needed a CT scan to learn more. As they ordered scans, the patient’s “sister” walked in. “Is that safe for the baby?” she asked.
“If she’s not doing well, the baby’s not doing well,” the physician in charge explained. “If we can fix her, the baby will be better off.”
Because this was a simulation, the results of the scan were immediate: Schertzer, now playing the role of a radiologist, announced that the patient had an injured spleen, requiring her to stay in the ICU for observation. The patient would not deliver her baby just yet.
“You don’t have time when someone is critically ill to work out your systems and communications.”
Kimberly Schertzer, MD, an assistant professor of emergency medicine
Emergency physicians, trauma surgeons, obstetricians, neonatologists, obstetrical anesthesiologists, obstetrical nurses and emergency nurses together designed the pregnant-trauma-victim simulation.
All the obstetrical residents, most of the emergency residents and many nurses in both specialties participated in the exercise. They didn’t know the test results beforehand: They had to consider various diagnoses and discuss the possibility that the patient would need to deliver the baby immediately.
In a real trauma situation, “You don’t have time when someone is critically ill to work out your systems and communications,” noted Schertzer, an assistant professor of emergency medicine.
The 15-minute exercises were video-recorded. Afterward, the participants watched the video and discussed their performance. The different specialists learned from each other.
The obstetricians now better understand the choreography of trauma medicine, including the primary and secondary surveys in which physicians check vital signs and then scan the patient for injuries. The emergency physicians were reminded not to keep a pregnant patient lying flat on her back; they also understand that lab results that appear normal are not necessarily OK for a pregnant woman.
Every few weeks or so, the department runs a simulation of a different treatment scenario, but it ran the pregnant-patient exercise 20 times from fall 2017 to March of this year. The team of clinicians from Stanford and Lucile Packard Children’s Hospital Stanford focused on it after research showed that pregnant trauma patients are more likely to die, possibly because clinicians are reluctant to run scans or even treat them for fear of harming the fetus.
Since running the simulations, Schertzer said, the relationships between obstetricians, radiologists and trauma specialists have strengthened. “It was a great project,” she said. “We really built a lot of bridges.”


A trial run
During a dress rehearsal before the new hospital opened, the emergency team enacted various scenarios. In one, Callagy, the executive director of emergency services, played a male car accident victim whose condition was so dire the Life Flight helicopter flew him to Stanford Hospital.
Her performance wouldn’t garner any acting awards: She may have been stretched out on a gurney, but she was more involved in her real role, answering texts and emails on her cell phone. Pointing to a nurse who was taking notes on an iPad, she said, “Write down that we need to check all the doors and make sure they open quickly.”
In separate cases, the team “treated” a psychiatric patient with violent tendencies and a patient who needed dialysis.
While the attending physician listed the accident patient’s vital signs, a nurse adjusted the light over the gurney, and a technician rolled a chest X-ray machine into the room. Everyone accompanied the “patient” to the CT scanner room, then to the elevators that would take him upstairs to an operating room.
During the drill, team members frequently stopped to discuss how they could save time, where they would direct family members, who would retrieve blood. Because everyone was dressed mostly in scrubs or street clothes, it was difficult to tell who was a technician, a nurse or a physician, but everyone asked questions and offered solutions, stepping outside their real-life roles to address problems.
It was the kind of collegiality that encourages Mahoney. “We’re seeing a flattening of the hierarchy,” she said. “We want to be an organization where everyone is heard and everyone is valued.”

