Tomorrow’s hospital today
Advanced technology and a design that puts well-being first come together in the new Stanford Hospital

There’s a line that David Entwistle, president and CEO of Stanford Health Care, recalls hearing his colleague George Tingwald, MD, say on more than one occasion: “The future is not what it used to be.”
Tingwald’s quip refers to the potentially mind-warping challenge of planning a hospital meant to serve for at least 100 years. That building, the new Stanford Hospital, opened its doors Nov. 17.
Online extra videos
Videos showing construction on the new Stanford Hospital, and more.
“You future-proof a building by trying to understand how to create the most flexible framework to allow for change, even though you may not know what that change is,” said Tingwald, who is Stanford’s administrative director of medical planning, as well as an architect and a surgeon.
The result of all this planning, which called on the expertise of hundreds of clinicians, staff and community members, is the seven-story, light-filled building designed to promote healing and facilitate teamwork among staffers and clinicians.

The building — the largest on the Stanford campus at 824,000 square feet — was built to withstand an 8.0-magnitude earthquake and can double or even triple its patient capacity in the event of a disaster or mass casualty event. It has its own sewer tank, water tank and generators that can produce 2.5 megawatts of power.
Within its walls, advanced technology; highly skilled, compassionate staff; and patient rooms with picture-window views of nature come together to make an outstanding setting for medical care, research and education.
“The new Stanford Hospital presents unprecedented opportunities to transform care,” said Lloyd Minor, MD, dean of the Stanford University School of Medicine.
“It’s a beautiful, serene setting for healing that is also an advanced incubator where we can cultivate our vision of precision health — predicting and preventing disease in the healthy and precisely diagnosing and curing disease in the ill. For patients and families as well as medical students, trainees and scientists, the new Stanford Hospital promises to raise the bar for all we do in care, research and education.”
Future design to help patients flourish
The motivation to build a new hospital came from stringent seismic safety requirements set by California in 1994, and from the need to increase capacity to serve a ballooning San Francisco Bay Area population.
Into its operations are woven about 180 applications that make the hospital a working laboratory for health care technology — including patient-comfort controls at every bedside to adjust lighting, room temperature, window shades and entertainment, and two units equipped with artificial intelligence-enabled cameras to study how monitoring can improve quality and patient safety.
Wheeled robots will transport linen and refuse, so people won’t have to. Heart-rate monitors, oxygen saturation monitors, infusion pumps, automated prescription-filling machines and hand-held devices used by nurses and doctors are connected to patients’ electronic health records that are updated in real time.
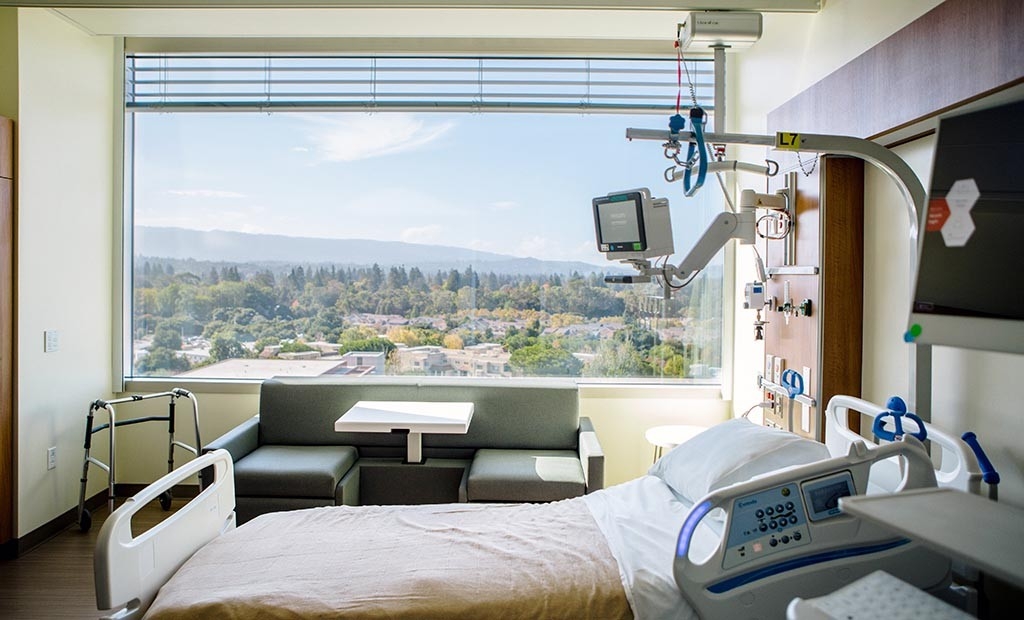
Artwork and nature’s beauty are visible throughout the hospital — 4 acres of gardens, views from every patient room, wall-to-wall windows in common areas and dramatic artworks that delight and inspire. The emphasis on art and nature reflects the growing recognition that they contribute to healing and well-being.
“From the patient rooms, the views are spectacular,” said local resident Michael Moore, a member of the hospital’s Patient and Family Advisory Council who toured the new building before it opened. “You’ve got the mountains to the west, the skyline of Palo Alto to the east and campus — one of the greatest views of Hoover Tower. It’s absolutely beautiful. And then at night, when the sun goes down, in that pure light, it’s absolutely breathtaking.”

With the new hospital open, the older hospital next door houses the pediatric emergency department and the inpatient psychiatry unit, and a section is being renovated to become a cancer hospital. The two hospitals, which together hold 600 adult beds, are joined by a bridge spanning an outdoor pedestrian promenade.
The new hospital, designed by a team led by Rafael Viñoly Architects, is built on base isolators — a structural foundation decoupled from the building it supports — to allow the structure above to remain steadier during an earthquake, versus making the entire building fixed and rigid. That early decision opened the door to the building’s architectural potential. The $2 billion project is the result of more than a decade of work, including six years of construction.
Coming through the new hospital’s front doors, patients and visitors find themselves in a wide-open, circular atrium topped with a soaring glass ceiling. Incorporating natural light and large windows with views guided the planning process from the beginning, said Tingwald. “There is daylight and a view within 50 feet of any point in the building. Every corridor ends in a window.”
Patient rooms are on the top four levels of the hospital, where four towers extend out from the center of the building. Each of the 368 rooms has a single bed and wall-to-wall picture window showcasing views of the Stanford campus and foothills. And each has a bathroom and a daybed for visitors.
Bringing the building to life
The focus for Alpa Vyas, vice president of patient experience for Stanford Health Care, is not so much on the building, but on the people within it.
“The real task for our team, as we were getting closer to opening day, was how do you kind of breathe life into this beautiful, amazing building?” she said. “It’s really the people within the building who bring it to life. The experience is not only the physical facility and the environment, it’s also the culture and service.”

Beyond the floors dedicated to patient care and procedures, the new hospital’s third floor is devoted to cultivating wellness. The floor features lounges for patients and their families, a lounge for staff, a dining area, a meditation/chapel space, and access to outdoor gardens and a walking trail. It also has a health library and caregiver resource center.
The goal is to build a knowledgeable network of people to support patients and their families long after they leave the hospital, Vyas said.
“How do we care for these individuals as well, not only their health, but also their knowledge and understanding about the future of the disease or diagnosis that their loved one is dealing with?” she asked. “How do we empower them to be the extension of Stanford when it comes to helping their loved one?”
The patient navigation team members are available to explain resources that add to the ability of family or friends to support the patient’s successful care, even from a distance. One of those resources, MyHealth, an app that Stanford patients have used for several years to manage their care and medical information, has been updated with new features. A “hospital view” feature activates as soon as patients are admitted, guiding them through their stay using navigation tools and content elements that keep them, and others they designate, informed about their care.
“Family members may be in a chair right next to the patient, or they may be 3,000 miles away,” Vyas said. “A daughter who lives in Washington, D.C., can keep tabs on what’s happening with a parent who may be hospitalized.” The daughter could also learn about the parent’s transportation needs upon discharge from the hospital.
Interactions with patient navigation experts add an important layer of personal care to continuing advances in medicine. “There’s a balance between future innovation, technology and the human touch,” Vyas said.
The future we know
Building a hundred-year hospital means understanding the future in two ways, said Tingwald. “There’s one category, the future you know, and then there’s this whole category of the future you don’t know. And we tried to respond to both of those.”

Emergency department planners learned from events like 9/11 that they need to be able to rapidly scale up to accommodate more patients after a disaster or mass casualty event.
“You have to plan for today, but also for this enormous contingency,” said Tingwald, while noting that it wouldn’t be cost-effective to design a disaster-ready hospital that on an average day would be relatively empty. The difference in scale between the single patient and multiple patients — doubling or tripling the hospital’s capacity — is the critical ingredient of smart, future-ready design.
As the only hospital on the San Francisco Peninsula verified as a Level 1 trauma center by the American College of Surgeons — and one of only five ACS-verified Level 1 pediatric trauma centers in California — Stanford’s Marc Andreessen & Laura Arrillaga-Andreessen Emergency Department is equipped to handle worst-case scenarios.
“We are not the emergency room of sniffles,” said Alison Kerr, RN, chief administrative officer of clinical operations. “We see the transplant patients, the cardiac surgery patients, the trauma patients. These are our patients.”

The new emergency area is 2½ times the size of the existing department. The length of a football field, it has 66 large, private bays — each with the equipment necessary to accommodate at least one extra patient.
Four full, private triage rooms are equipped with exam lights, oxygen and full-size gurneys so patients can be treated in those spaces if necessary. New features include a dental emergency room and 55-inch, two-way video monitors near the foot of every patient’s bed for services that include both remote consultation services and medical translation for the hospital’s many non-English-speaking patients.
The adjacent 900-space parking structure can, in the event of a mass-casualty event, double as a triage center, with emergency showers and eye wash stations. Patients who arrive by helicopter at the touch-down space on the roof are quickly taken to a nearby elevator that whisks them straight down to the emergency room.
“The point A to point B is much quicker — a direct line,” said Kerr. For time-sensitive conditions like stroke or trauma, the moments saved can make a life-saving difference.
“It’s not just curing or caring for someone’s incision. It’s caring for the whole well-being, the spiritual, the emotional, the family,” Kerr said. “That’s reflected not only in the architecture, but the nature, the natural elements of light and greenery, that to me, as a nurse, are part of a holistic healing framework, peace and tranquility, not just for our patients and their families, but also for our teams.”

The future we don’t know
The plan for the intensive care and acute care units allows the possibility of one to be converted to the other over time. And an “interventional platform” has been built on the second floor, dedicated to diagnostics, procedures and surgeries of all kinds. The 3½ acres of space includes 28 operating rooms — among them nine hybrid surgery suites equipped with fluoroscopy units, which use X-rays to obtain real-time moving images during operations. Two of the ORs connect directly to an intraoperative MRI.
To understand what makes the interventional platform so advanced, it’s important to understand how things worked in the past, said Sam Wald, MD, associate chief medical officer for perioperative and interventional services.
At the older hospital, operating rooms and catheterization labs, where providers do image-guided heart or gastrointestinal tract procedures, for example, were all in separate areas. Patients who needed a combination of services received them independently of each other.
“We have both inpatients and outpatients who need extremely complex procedures, performed by multiple doctors from different services,” said Wald, who is also vice president of inpatient perioperative services.
In the new Stanford Hospital, he said, “doctors from different specialties can work together at the same time on the patient, with a single anesthetic. Our new interventional platform allows all of those things that are usually housed in separate spaces to be all in one place.”
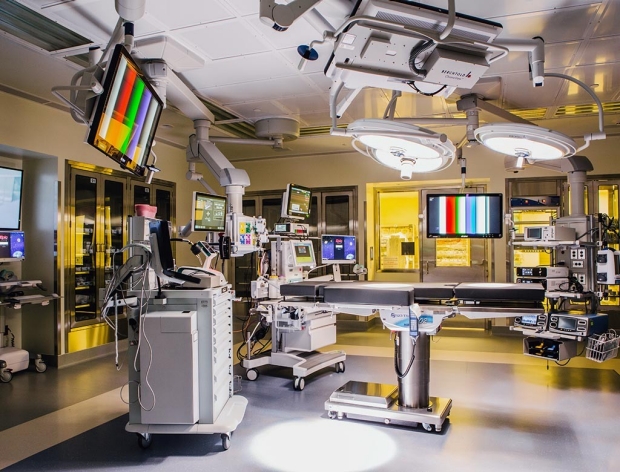

“Our faculty gave up their own personal silos to come together because they understood the value of working together,” Tingwald said. “It was really, really important, both operationally and from a design standpoint. Now that it’s done, it seems so intuitive. Like, how could people work any other way? Well, a lot of the world is still working any other way.
“In traditional hospital planning, you’d say, ‘Well, I know that an ophthalmology room needs to be this big. And that a gynecology room needs to be this big and a trauma room needs to be bigger and an open-heart operating room needs to be bigger than that,’” Tingwald said. “And you’d end up with five or six or seven different size rooms, responding to the traditional square footage for each of those procedure types.”
“Our faculty gave up their own personal silos to come together because they understood the value of working together. It was really, really important, both operationally and from a design standpoint.”
Procedures change dramatically over time, Tingwald explained, and many that once required fully opening a patient’s chest, such as heart valve replacement, can now be done through a small opening in the skin, where a catheter tube, laparoscope, endoscope or robotic device can be inserted.
Still, that doesn’t mean the space needed to perform such surgeries is smaller: Advanced equipment often takes up more space, and it’s hard for surgical teams to work — and teach — in tight spaces. Small rooms, therefore, become obsolete quickly.
The demand for bigger rooms is only growing, Tingwald said, so he planned for that: “We have all big rooms,” he said, “and they’re all the same size.”
The decision has a surprising advantage, he said, because surgeons will usually choose to operate in a larger room over a smaller one. Plus, space is needed for new equipment and technology.
“So when they’re all large, everybody has access to the same size rooms,” Tingwald said. “Some might say, ‘Why are we building all big rooms? Doesn’t that cost more money?’ At the end of the day, it is a savings because of the flexibility it provides.”
Supporting the patient
In many cases, the futuristic technology of the new hospital also makes way for more meaningful human interactions, offloading tasks that can be automated so caregivers have more time and patients are interrupted only when necessary.

“Imagine maybe concentric rings, where the first ring is technology that the patient experiences directly,” said Gary Fritz, vice president and chief of applications. “Then one ring out is technology that’s used by clinicians to take care of the patient. And in the next ring further out, there’s technology that supports the hospital, which supports the people who are taking care of the patients.”
It’s easy to imagine those rings separate from each other, but in fact most of the technology they illustrate is deeply interconnected. The system that’s wired through the walls, ceilings and a multitude of medical devices in the new hospital is wirelessly connected, for example, to secure hand-held devices for the care team and for patients.
The same MyHealth app technology that prepares and guides patients throughout their stay also gives care teams seamless access to patients’ electronic health records.
“Our care team members check in and check out for their shifts in our electronic health record system,” said Fritz. “So we actually know who’s taking care of patients at any given moment in time. What we’re doing is exposing this to the patient, demystifying the experience for patients who may wonder who they’re talking to or who is taking care of them.”
Technology also gives patients more control over their environment: They can use a bedside tablet — or their own device — to control the lighting, temperature and window shades, and to order food. They can also request such services as music, a massage or a visit with a therapy dog. The video monitor at the foot of every bed can display educational programming and entertainment.
And, in a major technological leap, their electronic health records are automatically updated with each new medical activity, relieving providers of the burdensome task of manually updating the records. In addition, telemetry systems record data from any device linked to the patient, such as a heart-rate monitor, an oxygen saturation monitor or an infusion pump, which delivers controlled amounts of fluid medication or nutrition.
Supporting those who support the patient
Traditionally, many hospital devices have audible alarms that alert a nurse to check the patient or the device. But alarms disturb a patient’s rest and sometimes go off when there’s nothing of concern. “There are published reports showing that about 72% to 90% of these alarms are false,” Fritz said. “So we’re changing the way alarms are presented to make them easier to identify and address.”
The alarms and alerts will also no longer be audible in patient rooms. Instead, providers will get immediate notifications on a hand-held device, called a Voalte or Connect phone, that they carry with them. Providers can review and respond to the alerts accordingly, and in some cases handle the issue through the devices, without disturbing the patient.
Besides providing alerts and allowing for phone calls and text messaging between colleagues, the devices have a staff directory, provider availability information and access to patient health records. At Stanford Hospital and Lucile Packard Children’s Hospital Stanford, 2,200 of the devices have been distributed.
“We’re using technology to deliver better services in ways that won’t upset patients or interrupt their recovery process,” Fritz said.
Fritz described the integrated electronic system used at the new hospital as an example of the “internet of things” — known in tech as simply IoT — in which devices are interconnected and able to automate the transfer of data. “This is an IoT hospital of the first order,” Fritz said.
Sensors in every biomedical device and most of the laptops and other equipment are also connected to a real-time location system throughout the hospital, allowing for more accurate inventory and servicing, and, ultimately, the need for fewer devices because they’ll be better managed, Fritz explained. The system is also linked to employee badges, so when doctors or nurses call for assistance, they need only press a button on their badge to alert other staff or security of their location.

Supporting the hospital
Getting things from one place to another in the new hospital has also stepped into the future. Twenty-three wheeled robots with mapping sensors are on deck to deliver linen and other materials.
And in a first-in-the-world integration, the new Stanford Hospital pharmacy will have a secure system using three robotic machines that select medications and prepare them into single doses to be delivered to one of 115 medication-dispensing stations throughout the new hospital. Best of all, the order can be placed directly in the patient’s electronic health record, which monitors returned medication, too.
“It’s an integrated pharmacy supply chain system with a single inventory,” Fritz said. “So we know if a medication dispensing station is getting low on drugs; it actually communicates with the robot that automatically replenishes it. And if the robot’s supply is getting low, it automatically sends an electronic message to the people who manage our supply chain, who then communicate electronically with the distributor or manufacturer. And we get it replenished automatically.”
Being able to return unused medication is a great leap forward, Fritz explained, because throwing away medications is costly and potentially hazardous to the environment. “We’ve taken our medication waste — our throwaway — down to lower amounts,” he said.
The new hospital still employs a 120-year-old, tried-and-true delivery system — pneumatic tubes — to deliver tissue and blood samples and other medical materials more quickly and efficiently than any other way. In the system, foot-long cylinders shoot through tubes to stations throughout the hospital, powered by vacuum pressure. The new hospital adds 4 miles of tubing to the 4 miles in the older hospital building.
“We’ve designed the new Stanford Hospital to be a great place for patient care,” Fritz said. “But it’s also a platform for the next generation of medical innovation, and for teaching the next generation of physicians.”
Minor agrees. “Through transformative discoveries, the education and training of future health care leaders, and innovations in predicting, preventing and curing disease, the new Stanford Hospital’s future-focused environment will surely have an impact that reaches far beyond our campus.”
“This combination of beauty, space, capacity, capability, technology and timelessness — I’m not sure how many places have that combination all in one. It’s a renaissance hospital.”
Sam Wald, MD, associate chief medical officer for perioperative and interventional services
Advisory council member Moore and his wife, Lynn Fraher, had their first glimpse of the new hospital’s construction in 2013 after he had a heart procedure and his doctors urged him to move around. As the couple wandered through the hospital hallways they noticed a big hole in the ground outside one of the windows.
As his health improved, they watched the building come to life. Moore had many Stanford Hospital stays over the years: In 2000, he was diagnosed with hepatitis C, and in 2007 he received a liver transplant and heart valve replacement in a back-to-back surgery.
These days they have a whole new relationship with Stanford Health Care. After more than 10 years of volunteering with the hospital — as patient advocates and on the advisory council, which Fraher led for four years — Fraher became a hospital employee last year in patient relations. In October 2019, she became a patient navigator in the new family and caregiver resource center.
For Entwistle, it’s not the hospital that raises the bar for staff members like Fraher, but the other way around.
“The new Stanford Hospital is a setting worthy of our incredible physicians, nurses and staff,” Entwistle said. “We’ve created an environment to match the high caliber of the care they provide, while offering patients and families an atmosphere that has been designed to promote healing at every step.”
As Stanford Health Care’s staff, patients and families explore and feel at home in the new space, they’re also learning that it’s unique. “This combination of beauty, space, capacity, capability, technology and timelessness — I’m not sure how many places have that combination all in one,” said Sam Wald, MD, who oversees the interventional platform. “It’s a renaissance hospital.”
George Tingwald talks with Paul Costello about designing the new Stanford Hospital to be one of the most technologically advanced hospitals in the country.
Alpa Vyas she discusses how her patient experience team works to ensure that the new hospital reflects a culture of wellness and balance between new technology and the human touch.
Gary Fritz discusses what it took to build the hospital of the future and how the technology at the new hospital is designed to support both the care team and patients.

