Expressions
Medical students creating art

The role of art in medicine, at first glance, can appear amorphous, indistinct, even at odds with the basic tenets of science. And yet, the arts remain essential to that same human condition to which health care providers dedicate their lives — and they are key to the creativity of science.
At Stanford, about half of all medical students become involved with the arts and humanities through Medicine and the Muse, a program that integrates the arts and humanities into medical education, says Audrey Shafer, MD, director of the program and professor of anesthesiology, perioperative and pain medicine. About a dozen each year receive funding through the Stanford Medical Scholars Research Program to pursue MedScholars projects focused in the arts.
“The practice of medicine is a human endeavor,” Shafer says. “The arts enable us to think more critically about what medicine is and who we are, as well as helping us to understand the perspective of the patient, to have empathy for people who are ill.”
And, as you’ll read, the arts can play a role in helping to heal the healers themselves.
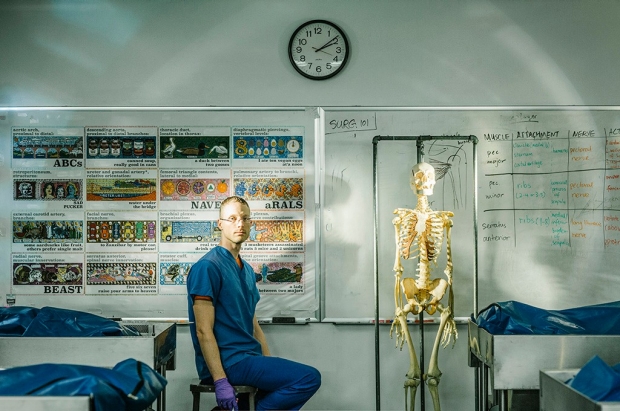
The graphic artist
The tall, fast-talking, blue-scrubs-wearing Nick Love leans closely into the whiteboard in Stanford’s clinical anatomy dissection lab, where he’s hung a poster-sized rendition of his multimedia illustration, titled Sixteen Anatomic Mnemonics.
Love has drawn upon his skills as a graphic artist and former medical illustrator — using graphic design software combined with hand-painted splashes of color — to create a work of art as his MedScholars Project. Sixteen Anatomic Mnemonics is an illustration that both entertains and serves as a memory aid. It exists in various forms: online, as a book and, now, as a poster.
To each version he likes to add touches of something new.
“I like to give a one-off artistic feel to the piece,” says Love, a medical student who has already earned a PhD in developmental biology, as he dabs short brushstrokes of white paint into the spaces between the 16 boxed illustrations on the poster board.
Sixteen Anatomic Mnemonics is decorated with brightly colored illustrations of 16 medical mnemonics, the whimsical expressions that share the same initial letters as the lists of body parts medical students must memorize. There are Andy Warhol-inspired Campbell’s-style soup cans that spell out the branches of the descending aorta: celiac trunk, superior mesenteric, renal artery, gonadal artery, inferior mesenteric, common iliac (canned soup, really good in cans). And tiny toilet-sitting versions of Rodin’s The Thinker contemplate the rotator cuff muscles of the mnemonic SITS: supraspinatus, infraspinatus, teres minor, subscapularis.
The anatomy lab is where inspiration struck Love, as a first-year medical student. White-coated instructors would scrawl mnemonics across these same whiteboards, sing-songing the funny-bone-tickling memory devices for the edification of medical students.
Love chose 16 of his favorite mnemonics — most from his anatomy instructors, a few found online. He drew each one as a story within a story within a story that illustrates practical applications of anatomy. Visualizing these mnemonics could only help the memorization process, he figured.
Peer closely into the illustrated mnemonic for branches of the facial nerve: to Zanzibar by motor car, please! Then peer more closely at the words for the facial nerve branches, temporal, zygomatic, buccal, maxillary, carotid, posterior auricular, all illustrated with rainbow-colored Hot Wheels cars. And closer still, into the background where tiny Zanzibar maps float in space next to tiny floating faces, facial nerve branches sketched in.
“I like hiding things in all my projects,” Love says. “I’ve long been interested in the pop art movement, but I’m probably more of a science nerd at heart. In any case, I hope that my work will help people learn more about biomedicine.”

The dancer
Stanford medical student Amrapali Maitra joined the group of previously homeless and mentally ill women, many survivors of domestic violence, with trepidation. The exercise room in this shelter for homeless women in Kolkata, India, her new base for her anthropology research, was dark and dank. The group was mostly quiet, mostly sad, distracted or uninterested.
“I was nervous, but the music played and my body just sort of took over,” Maitra says. “I did what I like to do: folk movement, Bollywood dance, hip-hop. Everyone got so much joy from this. The women started clapping and laughing and dancing around. That opened me up to the worlds of these women.”
Morning after morning, these women who had escaped from violent homes, ending up first on the streets, then in the shelter, would find momentary comfort and healing through dance, Maitra says. The goal of her research, conducted in this shelter, was to explore experiences of domestic violence among poor and marginalized women in Kolkata. In writing about the experience, she explains how dance enabled her to connect with her research participants.
“Through dance, I formed attachments with the women, across steep barriers of class and cultural difference. Movement equalized us; we found harmony in beats, steps and silence.”
Indian dance has been a part of Maitra’s life since she was a little girl studying the classical form known as Bharatanatyam. It continues to be so now, both as a medical student treating patients and as a PhD student studying domestic violence in India. Like other medical students passionate about the arts, Maitra has woven her talent together with her skills as a writer, researcher and health care provider into a pattern that she believes will best lead to the healing of others.
‘Through dance, I formed attachments with the women, across steep barriers of class and cultural difference. Movement equalized us.’
“Dance is a thread that has always been there,” says Maitra. “It’s a way of seeing and being in the world. I see how it shapes my approaches as a physician. It permits a different kind of expression than oral narrative.”
A native of Kolkata, Maitra studied history and literature as an undergraduate at Harvard University, always knowing she wanted to be a physician. Her MedScholars project entailed developing and implementing a domestic violence screening tool in Dhaka, Bangladesh. She has since spent 16 months conducting research in India, where dance has played a key role in helping her to connect with and help heal abused women. In India, dance is a big part of everyday life, both informal and formal, Maitra says, so it was just a natural extension for her to use her skills in traditional Indian dance to reach out to her research participants.
“Certain things you can express through dance — feelings of rage, sadness, protest,” she says. “In the form of Indian dance I do, we are trained to express mood or emotions with the face and hands and body to show feelings of disgust or peace or anger or love. For me, moving with these women, I felt their pain, the abandonment and the abuse that these women have felt.”
The writer
During his surgery rotation in his third year of medical school, Matt Bucknor, MD, remembers standing by the side of a patient. He was dressed in the white coat of a physician, yet a nurse mistook him for a janitor. The experience was jarring, but not new, he says matter-of-factly.
“Implicit bias is alive and well. It touches every corner of our health care system,” says Bucknor, now an assistant professor of radiology at UC-San Francisco. While he was growing up in a diverse and tolerant Maryland suburb, and as an undergraduate at Harvard University, he says, racism had never felt like a barrier to his professional or academic development. As an African-American physician caring for patients, this changed.
And so he wrote about it.
For Bucknor, the art of writing, a passion that emerged just as he entered medical school, became a way to explore his experiences navigating the new world of medicine. Between rounds, whenever there were short breaks in the daily demands and long hours of medical school, he’d pause to jot down notes, fiddle with phrases.
“It renewed my energy,” says Bucknor. “Writing and communicating ideas helped sustain me in medical school and residency. It was a crucial outlet.”
His writings developed into a novel. He wrote the first third as his MedScholars project, then continued writing a 400-page first draft. The novel tells the story of Marcus, a young, black medical student in San Francisco confronting issues of race and identity while plunged into the physical and emotional demands of becoming a physician. Bucknor is still actively working on the book and also leads one of the Pegasus Physician Writers groups at Stanford.
Marcus’ words in the early pages of the novel could have been Bucknor’s own: I count myself among a lucky few, a black man in America who has seen hard living, but never known it.
He writes about what he knows, such as the sorrows of dealing with the death of your first patient as a medical student:
I waded into that awful inevitable moment like a toddler pushed into the center of a pool. I felt ashamed and embarrassed. Kayla’s death wasn’t my fault. But there is no way that mattered because all I could feel was that it was entirely my fault.
And the joys of knowing a patient will survive:
That is my favorite part of the job. Knowing that someone is going to be okay, before anyone else. That moment — it feels like catching a firefly that no one else can see.

The musician
At the still point of the turning world. Neither flesh nor fleshless;
Neither from nor towards; at the still point, there the dance is,
But neither arrest nor movement.
— T.S. Eliot, Four Quartets
Ben Robison is a musician. It’s part of who he is.
“For me, making music is like eating or breathing,” says Robison, a professional violinist with a doctorate in musical arts. Robison is in his fourth year of medical school and co-founded the Stanford Medicine Music Network, which brings musicians together to play music.
Together with Matthew Wetschler, MD, a painter and a third-year resident in emergency medicine, Robison is hoping to build a community of medical practitioners dedicated to what he calls “art-enabled reflective practice” — a foundation for reflection inspired by art.
Both men drew sustenance from their art during medical school. Painting and music provided this foundation for reflection, time away from the emotional strain from caring for the sick and injured. It rejuvenated them. And it helped to recharge their empathy, Robison says.
“Incredible health care workers in the ER and throughout the hospital take care of as many as 30 people a day,” Robison says. “People in extreme pain and distress. It is without a doubt a taxing job. You are busy being a doctor, a professional. It can be very analytic, with your time dominated by diagnosis, documentation, computers, treatments.”
‘His art, my music — it was and is an incredible way to process what goes on in the hospital, the wonderful and the terrible.’
There is little time for deep reflection.
“His art, my music — it was and is an incredible way for us to process what goes on in the hospital, the wonderful and the terrible,” Robison says. “We thought we could use the practice of art to inspire reflection and to offer shared empathetic experiences for health care providers — to heal those who heal others.”
With their MedScholars project and additional funding from Medicine and the Muse, Robison and Wetschler are planning to provide that sort of comfort to other health care providers, including physicians, nurses and technicians. They are organizing a tour of medical schools where they will present a two-hour concert and panel on art and wellness. They’ve also created a website, atthestillpoint.org, to support the tour — the name comes from a T.S. Eliot poem. The website is designed as a repository for pieces of artwork collected from health care providers. Their vision is to inspire reflective practice through both the appreciation and making of art. In the spring, they plan to take the show on the road, touring medical schools. Each event will include Robison improvising on the violin, a talk by Wetschler and a panel discussion, and will conclude with audience participation.
“Maybe it could be inspiring. Maybe it could help prevent burnout,” Robison says.
The project began with both of these artists posting their own artistic creations on the website — a Wetschler painting and a Robison musical composition. Their message:
“Here’s art. Be with art. Take that moment. As a musician our canvas is silence. Drop into that stillness and draw a line.
“Come from a point of stillness.”

The filmmaker
Slowly, the lesbian, gay, bisexual and transgender veterans tell their stories — of being set up for a date rape by a superior, of rejection by the military they love, of the little boy who looked like a little girl who always wanted to join the military. They talk about mental illness, suicide, post-traumatic stress disorder, nightmares, insomnia. And then they speak of the healing that occurs from telling these stories.
“I was a victim of military sexual trauma; I had PTSD early on,” says one of the veterans speaking in the documentary The Camouflage Closet. “I was considered a broken soldier. I was a target of military sexual trauma. I was told I would be ruined if I told anyone. I was naive. I was 19.”
In his first year as a medical student, Michael Nedelman, already an experienced filmmaker, began work on his MedScholars project: The Camouflage Closet, a documentary about LGBT veterans’ experiences with PTSD, trauma and recovery. The idea for the film emerged in a San Francisco arts workshop just before he began medical school, less than a year after the repeal of the policy on LGBT military members known as “Don’t ask, don’t tell.”
The film explores healing through vignettes in which nine veterans talk to the camera about prejudice, humiliation, violence and resilience. As a way of accessing often hidden memories, Nedelman provided the veterans with cameras and trained them to create their own video narratives.
“They were able to tell their stories on their own terms,” he says. “I think the camera might have played a big role in accessing these memories.
“I’ve been a filmmaker since I was 16 or 17 years old,” says Nedelman, who has an undergraduate degree in film studies from Yale University. One of his early works was Vision Voice, which explores the lives of three women living with diabetes and vision loss in East Harlem. His desire to tell the most accurate and compelling stories he could about health and medicine propelled him to apply to medical school.
His passion for telling true stories has since moved him into journalism. In 2015 he was awarded the Stanford-ABC News Global Health Media Fellowship, which took him to New Delhi to work on health campaigns, and eventually led to a position as a digital producer for ABC News’ medical unit. Currently he is working in Atlanta as a producer of health and medicine stories for CNN Health.
Nedelman, who is on leave from medical school, plans to return and finish his degree. “People don’t just learn about their health from their doctors,” he says. “They see something on TV, or they look things up online. We need doctors behind the curtains, pulling some of those levers, to make sure that health information is accurate and trustworthy.”

