‘These patients are really fragile’
An intensive care team takes on COVID-19
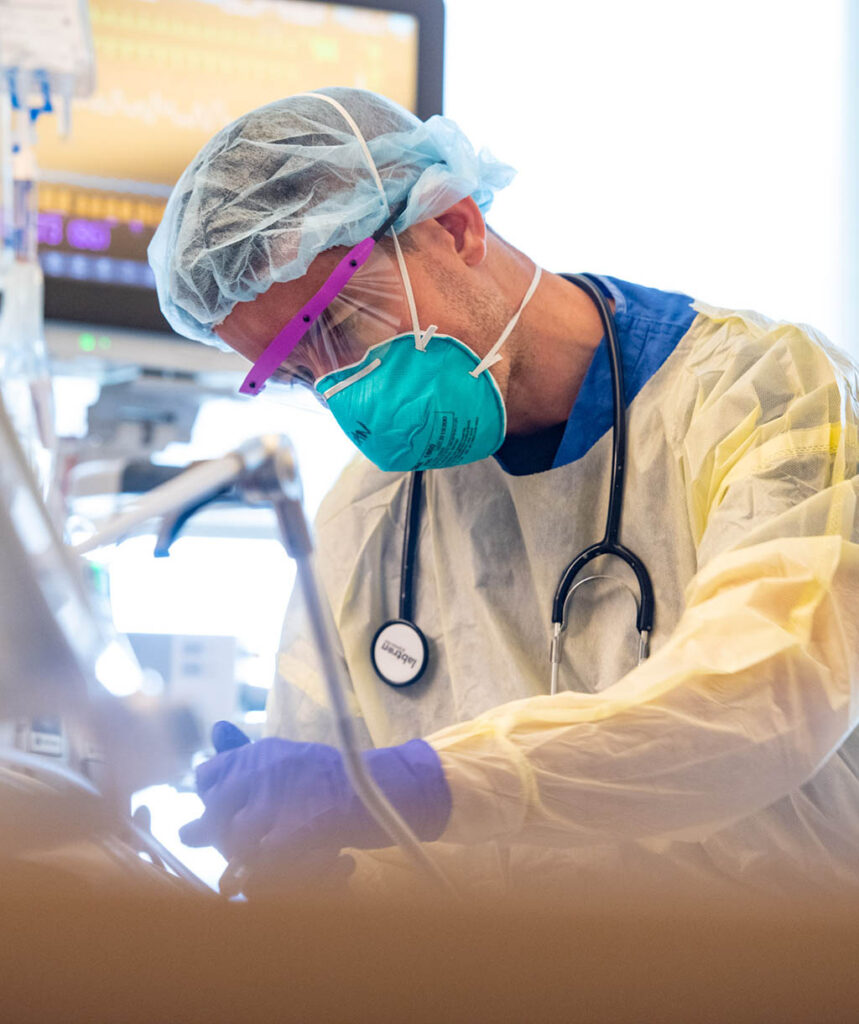
The first coronavirus patients to arrive in the intensive care unit at Stanford Hospital were wheeled in on gurneys, sometimes struggling for breath, often with frighteningly low levels of oxygen circulating in their blood.
They were pale and scared. Because visitors were barred to contain the spread of the virus, no family members were there to support them, and it was up to the ICU team to make life-or-death decisions fast.
This was early March, just before the World Health Organization declared the coronavirus outbreak a pandemic, and no one was sure how best to treat patients with this extremely infectious disease.
Related podcast
No one on the ICU had cared for patients with this illness before. There were no standardized treatment guidelines, and very little reliable research existed. Mostly, there were just rampant rumors of high mortality rates and even higher levels of contagion. The ICU team had to start from scratch.
“It was nerve-wracking,” said Dwayne Free, one of the frontline respiratory therapists, whose job is to help keep patients with infected lungs breathing. “There were so many questions around how the virus was spread. People were scared. Were there going to be enough ventilators? Enough personal protection equipment? Are we doing everything right?”
During the following months, the ICU team adapted daily to the ongoing crisis that has refused to subside. They’ve watched and learned from their patients while keeping up with an influx of new research from around the world.
From the beginning, the ICU formed a task force, bringing in Stanford colleagues to debate and create guidelines for the care of people with COVID-19. The guidelines are posted online and are continually updated in response to ever-changing news about the coronavirus.
It’s been a grueling time for the health care workers, but not without rewards.
“For those first couple of patients who made it out of the ICU after 30 or 40 days, everyone — nurses, respiratory therapists and doctors — lined the hallway,” said Maureen Fay, a registered nurse and director of clinical services for Stanford Health Care, who talks about the deeply felt camaraderie that has been forged among the ICU staff. “They were cheering. They were so proud.”
Urgency for collaboration
became clear
Chaired by Angela Rogers, MD, the Stanford COVID-19 critical care task force met three times a week at first to hash out the best-practice guidelines. At its peak during those early days, staff members were caring for 10 to 15 patients and preparing for the possibility of a sudden increase along the lines of what hit New York and Boston.
“Right away we knew we had to work together as a team,” said Rogers, an assistant professor of pulmonary and critical care medicine. “It quickly became evident that aspects of COVID-19 care were really different from anything we’d seen before. All voices needed to be heard. The respiratory therapists, nurses and pharmacists were crucial to the task force. They knew what could and couldn’t be done, and what was safe to try.”

This multidisciplinary team — composed of 50 health care workers, including physicians from a variety of specialties, nurses, respiratory therapists and a pulmonologist from Stanford Health Care – ValleyCare — met in the early morning.
They reviewed and debated reams of research gathered through after-hours internet searches. Some called colleagues in New York or Italy, where hospitals were treating large numbers of COVID-19 patients, for advice. They shared what they knew from their own ICU experiences, and what they were learning from treating COVID-19 patients.
“We wanted a way to add some scientific rigor to the decision-making process,” said Javier Lorenzo, MD, a clinical assistant professor of anesthesiology.
At first, what little was known about severely ill patients came from China, where the outbreak began, said Norman Rizk, MD, who until mid-September served as medical director of Stanford Health Care’s intensive care unit. But the enormity of what they didn’t know kept the team up at night. How was the virus spread? What supplemental oxygen methods were best? Which medications would help keep their patients alive? What was the level of contagion risk for frontline health care workers? They needed to find answers, and do it quickly.
“Should we give steroids?” Rizk said as he listed some of the many questions debated, sometimes fiercely, during task force meetings. “Who belongs on ventilators? Do we put our own most vulnerable care workers at risk at the bedside?”
Similarities with acute
respiratory distress syndrome
While a lot was unknown about COVID-19, scientists did know it was caused by SARS-CoV-2, or severe acute respiratory syndrome coronavirus 2. They knew the virus attacked the lungs, causing inflammation and infection, and reducing oxygen to the rest of the body. But the details remained unclear.
“We knew this was very similar to another condition called ARDS — acute respiratory distress syndrome — something that has been studied for 50 years,” Rogers said. ARDS causes fluid to collect in the lungs’ air sacs, depriving the body of oxygen. It, too, can be fatal.
“With ARDS, we often intubate and use ventilation to protect the lungs and allow them to heal,” she said. During intubation, a breathing tube is inserted through the patient’s mouth and into the airway. The tube is then attached to a mechanical ventilator that pumps air into the patients’ lungs, basically breathing for them.
Because they knew COVID-19 could quickly progress to respiratory failure, the plan early on was to follow the advice from China and not delay intubation, but do it early, as they might with ARDS. As the weeks passed, though, they learned that there were many differences between these two diseases.
Firsthand experience showed it was better to postpone intubation and ventilation for as long as possible. They saw that COVID-19 patients produced thicker, more problematic secretions that blocked the airway and frequently needed to be suctioned out.
“I’ve seen a patient who looks fine — they’re sitting up on their phone texting — then three hours later we’re intubating them to keep them alive.”
Jacqueline Hayes Albarran, a clinical specialist and respiratory therapist
When these patients could no longer breathe for themselves and ventilation was needed, they often were on the machine for unusually long periods of time. With ARDS, a patient might be ventilated for four or five days, Rogers said. But COVID-19 patients were sometimes ventilated for weeks at a time. And, surprisingly, most often they still survived.
“Sometimes patients show progress, come off the ventilator, and then need to go back on,” said Jacqueline Hayes Albarran, a clinical specialist and respiratory therapist, who emphasized how difficult it can be to predict an outcome because this is a new disease. “I’ve seen a patient who looks fine — they’re sitting up on their phone texting — then three hours later we’re intubating them to keep them alive.”
Thousands of unvetted research studies quickly flooded the internet, sometimes helping the team make treatment decisions, sometimes generating more questions. Should they be using experimental drugs, like remdesivir or hydroxychloroquine, which was reportedly being used successfully in other countries? Because inflammation is common in COVID-19 patients, what about using more steroids to tamp down the immune system? Because blood clots are a serious concern, should higher doses of anticoagulation medication be considered?
“Among physicians, there is always a strong desire to do something rather than nothing,” Rogers said, especially when treating a patient who may be dying. Still, the best option is often to do less rather than more, she said. The goal became to wait for clear evidence, whenever possible, before changing practices.
“First, you do no harm,” she said. “As we start reaching for therapies, we have to remember these patients are really fragile.”
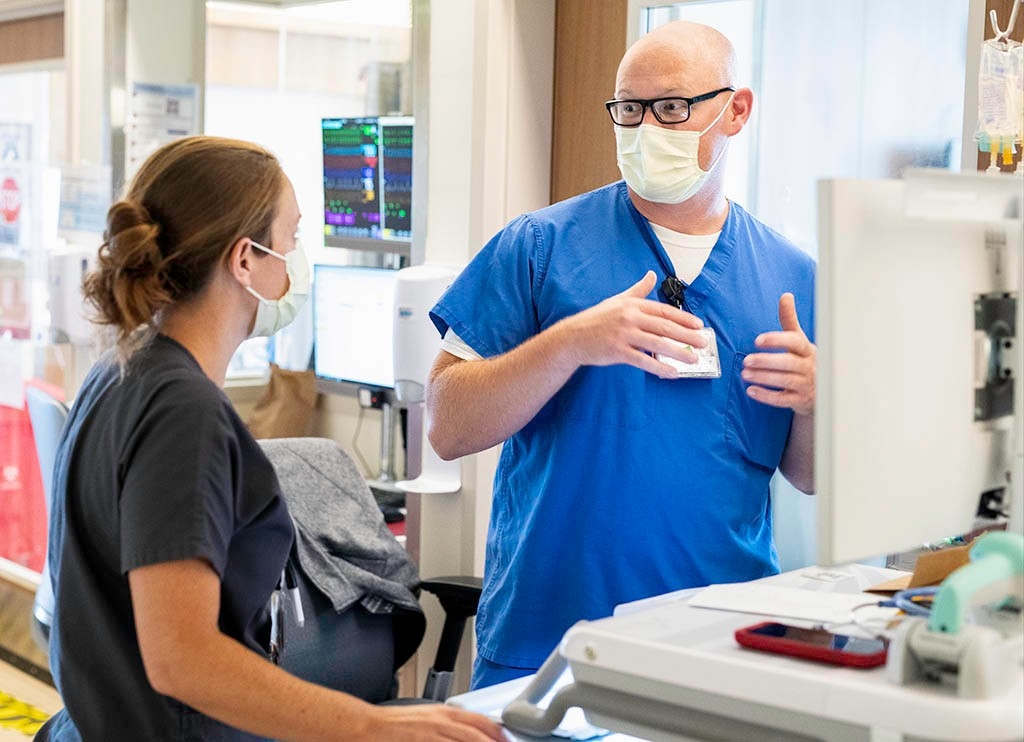
Few COVID-19 patients hospitalized
A small percentage — approximately 10% — of coronavirus patients at Stanford ever see the inside of an ICU, Rogers said. Most at Stanford are treated on the wards and sent home to mend.
Those who end up in the ICU are usually admitted because their organs are failing to the extent that they need round-the-clock expert care. The virus can cause multiple organs to fail, from the lungs and kidneys to heart or even brain. “It’s a crazy disease,” Rogers said.
Most ICU patients are given high levels of supplemental oxygen, which is supplied through a face mask or a tube inserted into the nose. If their condition continues to deteriorate, they are placed on a ventilator through the mouth.
In patients with prolonged respiratory failure, a breathing tube is inserted surgically into the neck because it’s more comfortable for the patient and requires less sedation.
The goal is to keep oxygen pumping into the body as long as it takes for the lungs to recover. Using a ventilator gives the body time to heal — to clear infection and inflammation — until the patient is strong enough to breathe independently.
“Part of the problem was that these coronavirus patients who showed up at the ICU often didn’t look as bad as they should with the extremely low oxygen levels they were showing,” Lorenzo said. That made it hard to know when a more invasive ventilation procedure was needed. “We are still learning how the virus affects the lungs, just how diffuse the inflammation is and how it affects the transfer of oxygen. It really just creeps up on people.”

Once the decision is made to put someone on a ventilator, health care workers follow a strict protocol to protect themselves.
Any time spent in the room of a COVID-19 patient puts staff at risk of exposure, Rogers said, so the goal is to keep that time to a minimum while still providing the best possible care.
Caregivers are at risk, for example, if a patient coughs as the breathing tube for the ventilator is inserted, sending infectious droplets into the air, or if one of the circuits connecting the breathing tube to the ventilator comes lose, spraying air that’s been infected with the virus into the room.
Even touching a countertop is a risk. So the frontline workers must move cautiously, while also acting quickly to help a patient struggling to breathe and to minimize their own exposure.
Typically, three caregivers enter a patient’s room to insert a breathing tube: an anesthesiologist or critical care physician, a respiratory therapist, and a bedside nurse, each meticulously dressed in full protective gear — face mask, shield, gloves and gown, Free said.
They give the patients sedatives and paralytic agents to keep them calm and still, then a doctor slides a breathing tube down the windpipe into the lungs. The entire procedure normally takes about 15 minutes, but with the added steps to prevent coronavirus exposure it can take up to an hour.
A respiratory therapist at the bedside assists with the insertion of the breathing tube while also suctioning out lung secretions and checking that connections to the ventilator are safe and tight, Free said. The respiratory therapist and a nurse team up to reassure patients through what can be a frightening experience, he said.
“The hardest part for us is at the bedside,” he said. “You go in and see these patients in their most vulnerable state, really struggling to breathe, but right next door the same situation is happening. You try to keep them as comfortable and safe as possible. Then you have to just do your job, move on. I’d go home at night and talk about it with my wife. She’s a critical care nurse and could understand.”
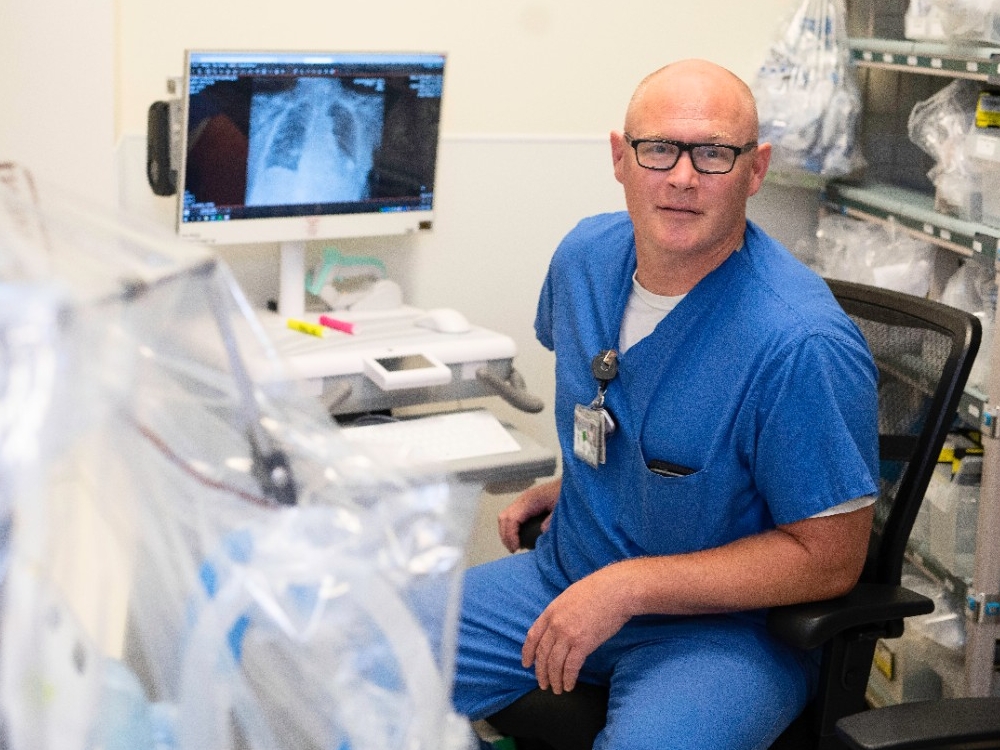
After each of these 12-hour shifts, Free returned home to his wife and daughter, always first stripping down in the garage and throwing everything into the washing machine. Fear of infecting families is a continuing stressor for these caregivers, Fay said, but it was especially strong early in the pandemic.
“They’d say, ‘I signed up for this, but my family didn’t,’” she said.
As time has passed, Free said that he now feels safer at work than anywhere else outside of his home. The safety protocols set up by Stanford have helped the ICU COVID-19 team have confidence that they are not only keeping themselves safe but they’re doing the best they can for their patients, Rogers said. Today, many of those early fears have been replaced by moments of success.
“Caring for these patients is really hard,” Albarran said. “But there have also been some heartfelt moments, like getting to speak to a patient after the breathing tube is removed. Hearing those first words that my patient has spoken in months, and for those words to be, ‘Thank you for saving my life,’ brought tears to my eyes.”
As more rigorous science came to light — with new COVID-19 clinical trials reporting results and peer-reviewed journals reviewing them — treatment protocols for Stanford’s ICU patients began to change.
After several large clinical trials showed positive results for the anti-viral remdesivir as a treatment for the virus, and there was a role for steroids in patients with more severe disease, clinicians adopted them as standard for care, Rogers said. When other studies showed that hydroxychloroquine didn’t harm patients but didn’t help them either, it was removed from the list of treatment options.
“We had a lot of meetings around these changes,” Rogers said. “In the early days, we were really flying blind, working hard to build a consensus based on our own team’s expertise and outside experts. It is exciting to see our standard of care continuing to advance in response to rigorous clinical trials. Every month of extra data helps.”
“We are still learning. We’ve seen enough patients to learn a lot from them, but it’s too early to say these will always be the best treatments.”
Angela Rogers, MD, an assistant professor of pulmonary and critical care medicine
Now the ICU’s treatment guidelines recommend steroid use for severe respiratory failure. Similarly, protocol now calls for higher doses of anticoagulation medication for coronavirus patients to protect against blood clots that have been shown to cause strokes, Rogers said.
“We are still learning,” she said. “We’ve seen enough patients to learn a lot from them, but it’s too early to say these will always be the best treatments.”
The team still meets once a week, with members spending their free time studying new scientific literature, sharing war stories with colleagues around the globe and learning from their patients at the bedside.
The frontline caregivers still sweat under their protective gear while reassuring frightened patients. The recovery rate for their ICU patients has continued to hover around 80% throughout the pandemic, Rogers said. And no health care workers have contracted the virus while working in the ICU.
“We still have adequate PPE because of heroic efforts in our supply line,” Rizk said in July.
By that time, the numbers of patients in the ICU had risen back to those highest levels seen early in May. A handful of state-mandated transfer patients from the Imperial Valley, where hospitals have been overwhelmed, are included in those numbers, but most are coming from the surrounding community.
“We are prepared again to surge if required,” Rizk said. “We have actually started a new ICU team that deals with just the COVID patients.”
“In late July, we rose as high as 14 patients in ICU with seven on ventilators. By late August, as numbers in the region are falling again, the ICU numbers had similarly fallen to eight with five on ventilators,” Rogers said.
No one’s sure why Stanford didn’t see a steep initial surge; perhaps spread of the disease was limited by early stay-at-home orders in the San Francisco Bay Area, or the fact that the patients tend to come from areas with low population density.
But patients with COVID-19 have not stopped coming, with some becoming severely ill and struggling to get better. So Stanford continues to prepare, responding to emerging data to provide the best care possible for each new patient, Rogers said.
“We learn from our mistakes,” said Lorenzo. “We refine our practices, try to make them a little bit more efficient. We rest. We take care of ourselves and our loved ones. We realize now that this is probably not going to be a peak, but a trickle of patients for a long time to come.”


