Upfront
A quick look at the latest developments from Stanford Medicine

In this Upfront package of articles, you’ll find updates on Stanford Medicine research about how mom’s voice improves a preemie’s brain, a tool for improving lost sight, and more.
Paddington for preemies
Hearing mom’s voice promotes language pathway development preemie babies’ brains, research shows
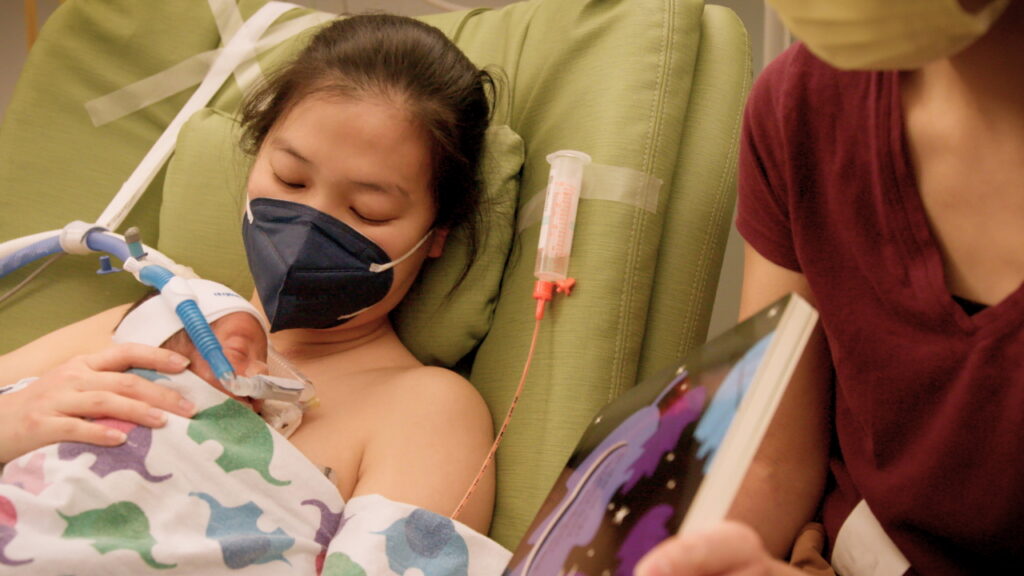
Hearing the sound of their mother’s voice promotes development of language pathways in a premature baby’s brain, according to a new Stanford Medicine-led study.
“This is the first causal evidence that a speech experience is contributing to brain development at this very young age,” said the lead author, Katherine Travis, PhD, an assistant professor of pediatrics at Stanford Medicine when the study was conducted, who is now on the faculty of Weill Cornell Medical School.
The findings were published Oct. 13, 2025, in Frontiers in Human Neuroscience. The senior author is Heidi Feldman, MD, PhD, the Ballinger-Swindells Endowed Professor in Developmental and Behavioral Pediatrics.
Premature babies are often hospitalized for weeks or months, during which time they hear less maternal speech than if they had continued to develop in utero. They are at risk for language delays, and scientists have suspected that reduced early-life exposure to the sounds of speech contributes to the problem.
Forty-six babies who were born more than eight weeks early were in the study. They were randomly assigned to a treatment group or control group. Over the course of a few weeks, babies in the treatment group heard recordings of their mothers reading the children’s book A Bear Called Paddington for 2 hours and 40 minutes every day. Members of the control group did not.
MRI scans were taken of the infants’ brains before they were discharged from the hospital. The images showed the arcuate fasciculus tracts on both sides of the brain, which contain bundles of nerve fibers that help process and understand sound. The left arcuate fasciculus is specialized for language processing.
The scans revealed that the language-processing pathway was more mature in babies in the treatment group than in babies in the control group. The right arcuate fasciculus was less affected by the treatment — a finding consistent with known differences in how the two hemispheres of
the brain process speech, the scientists said.
“Babies were exposed to this intervention for a relatively short time,” said study co-author Melissa Scala, MD, a clinical professor of pediatrics and a neonatologist at Lucile Packard Children’s Hospital Stanford. “In spite of that, we were seeing very measurable differences in their language tracts. It’s powerful that something fairly small seems to make a big difference.
Read the full story here
Help in sight
Help in patients with an advanced form of age-related macular degeneration are given back some sight in test of new device

A medical device invented by a Stanford Medicine researcher is the first capable of restoring functional sight to people with incurable vision loss, giving them the ability to perceive shapes and patterns, according to results published in October 2025 in The New England Journal of Medicine.
In a clinical trial, 27 of 32 participants with an advanced form of age-related macular degeneration, which destroys light-sensitive photoreceptors in the center of the retina, regained the ability to read within a year of being outfitted with the device.
The two-part prosthesis, called PRIMA, consists of a small, glasses-mounted camera that captures images and projects them via infrared light to a wireless chip implanted in the back of the eye. With enhancements enabled by the device, such as zoom and higher contrast, some participants could read with acuity equivalent to 20/42 vision.
“All previous attempts to provide vision with prosthetic devices resulted in basically light sensitivity, not really form vision,” said Daniel Palanker, PhD, a professor of ophthalmology and co-senior author of the paper.
Palanker first imagined a prosthetic device 20 years ago, when he worked with ophthalmic lasers used to treat eye conditions. “I realized we should use the fact that the eye is transparent and deliver information by light,” he said.
PRIMA provides only black-and-white vision, but Palanker is developing software that will enable the full range of gray scale, which is required for face recognition.
Read the full story here
Digital scientists
Researchers say it’s possible to work with AI-powered scientists to solve real-world problems

Stanford Medicine researchers have figured out how to create digital “scientists” that work together with minimal oversight to solve real-world biomedical problems. A paper published in July 2025 in Nature describes how a virtual lab of artificial intelligence-powered scientists devised a better way to create a vaccine for SARS-CoV-2, the virus that causes COVID-19.
Advances in agentic AI, collaborative systems of AI models that interact to autonomously pursue certain goals, enabled the creation of a virtual lab, said James Zou, PhD, associate professor of biomedical data science and co-senior author of the study. This gave him the idea to train these software systems to perform like top-tier scientists.
In the virtual lab, a researcher poses a scientific challenge to an AI principal investigator, or AI PI. “It’s the AI PI’s job to figure out the other agents and expertise needed to tackle the project,” Zou said.
For the SARS-CoV-2 project, the AI PI created an immunology agent, a computational biology agent and a machine learning agent. Another agent assumed the role of critic. Instead of proposing a traditional antibody, the AI team suggested a nanoscale fragment of an antibody.
A subgroup of researchers led by co-senior author John Pak, PhD, of the Chan Zuckerberg Biohub, created the nanobody and tested its ability to bind to one of the new SARS-CoV-2 variants — which is key to vaccine effectiveness — and found that it clung tightly to the virus.
Now, Zou and his team are analyzing the nanobody’s ability to help create a new vaccine and feeding the experimental data back to the AI lab to hone the molecular designs.
Read the full story here
Old mice, young muscle
An injection of a molecule involved in healing can turn back aging clock, study says

Some exercise and one injection of a molecule that’s part of the body’s healing process are all it takes to turn back the clock on muscle vitality if you’re over the hill. And are a mouse. Yet the discovery has compelling implications for people with age-related muscle loss or muscle-wasting diseases.
Stanford Medicine researchers determined that giving elderly mice a shot of prostaglandin E2, then allowing them to exercise on a treadmill over the next two weeks, dramatically increased their strength. The findings were published in June 2025 in Cell Stem Cell.
The research is the first to show that even a brief exposure to PGE2 rejuvenates muscle stem cells by erasing biochemical tags on their DNA that accumulate during aging and hamper the expression of genes involved in self-renewal, survival and muscle function.
An injection of PGE2 brokers the exchange in muscle stem cells of a lifetime’s worth of genetic markers for a new set of instructions that enhances the function of individual muscle stem cells and is passed down to their descendants.
“PGE2 is restoring the cells’ viability and ability to divide and rejuvenating their ability to regenerate and repair muscle damage,” said Helen Blau, PhD, the study’s senior author, the Donald E. and Delia B. Baxter Foundation Professor, and a professor of microbiology and immunology. “And it does so by inducing a heritable molecular memory.”
Read the full story here
Gentler cancer therapy
Using CAR-T cells a method of used for mRNA vaccines could boost curative effects
CAR-T therapy has been a boon for treating many blood cancers, but it’s onerous. Immune cells called T cells are removed from a patient, genetically engineered and then returned. Patients must also undergo a procedure to deplete their original T cells, leaving them at risk for infection.
A study led by Stanford Medicine researchers suggests a gentler alternative. Although the method has not yet been attempted in humans, it was safe and effective in laboratory mice, the study found.
The method generates CAR-T cells with the same technique used for mRNA-based vaccines: mRNA is delivered into cells where it spurs production of the desired protein — in this case converting ordinary T cells into CAR-T cells.
Unlike the suspension of T cells delivered in standard CAR-T treatment, the mRNA messages can be provided multiple times, amplifying its curative effects.
Tumors in 75% of mice with B cell lymphoma treated with mRNA were eradicated after several doses. The approach requires no harsh pretreatment to deplete existing immune cells, and it allows researchers to track where the modified cells are in the body.
The study was published June 10, 2025, in Proceedings of the National Academy of Sciences. Katherine Ferrara, PhD, a professor of radiology and chief of the Molecular Imaging Program, was the senior author.
Read the full story here
Pulmonary protection
Experimental drug could increase cell survival after exposure to toxin in wildfire smoke
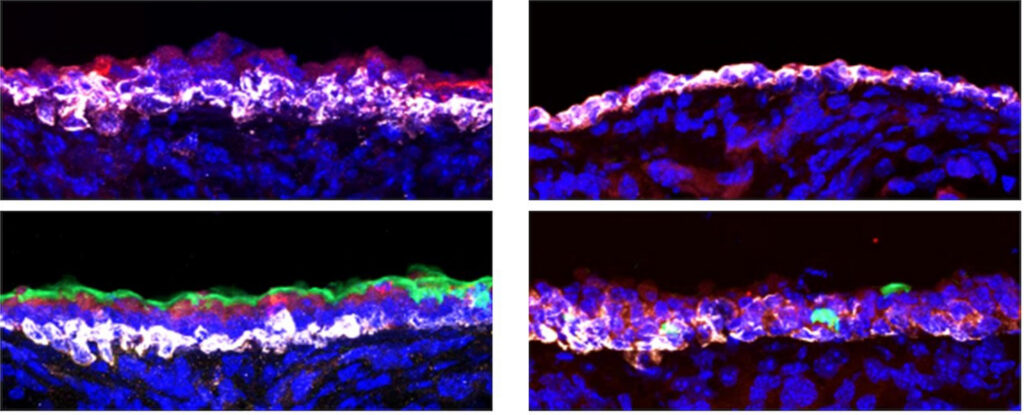
A chemical messenger named after a small, spiny mammal of the Arabian Peninsula protects lungs from toxic damage in mice and might play the same role in humans, according to a Stanford Medicine study.
Neuroendocrine cells, which combine the properties of nerve cells and hormone-producing cells, make the desert hedgehog protein in the trachea and pancreas. An experimental drug that activates the protein in mice initiated a cascade of biological reactions that dramatically increased cell survival after the animals were exposed to sulfur dioxide gas, a pollutant that mimics damage from toxins such as wildfire smoke.
In treated mice, 66% of ciliated cells, which use feathery “arms” to sweep particles and viruses out of the lungs, and 82% of secretory cells, which make mucus to trap unwanted invaders, survived. Only 9.7% of ciliated cells and 43% of secretory cells survived in untreated animals. A similar protective effect followed infection
with the flu or SARS-CoV-2.
Philip Beachy, PhD, the Ernest and Amelia Gallo Professor and a professor of urology and of developmental biology, was senior author of the study published in June 2025 in Cell. Scientists at University of California, San Francisco contributed to the work.
The researchers are studying how the hedgehog signaling pathway might be activated in humans to prevent lung damage in people who are exposed to airborne toxins.
Read the full story here
Surgery prehab in sight
One-on-one coaching improves prehabilitation success

Surgeons often urge people to improve their physical and mental health prior to surgery — known as prehabilitation — to reduce complications afterward. A new Stanford Medicine study shows that people prehabilitate more successfully with a little one-on-one help.
In the study, standard prehab patients received literature about exercise, healthy eating, stress reduction, mindfulness and cognitive training. Personalized prehab patients received twice-weekly online coaching on the same topics.
Within 30 days of surgery, 11 of the 27 standard prehab patients had moderate-to-severe post-operative complications, compared with four of the 27 personalized prehab patients.
Analyzing patients’ immune cells, researchers found reduced overreactivity in some immune cells and lower baseline inflammation in the personalized group — surprisingly large shifts for a low-cost at-home intervention, they said.
“It’s a measurable effect that you would expect from a pharmacological intervention, honestly,” said Brice Gaudilliere, MD, PhD, a professor of anesthesiology, perioperative and pain medicine and a senior author of the November 2025 study in JAMA Surgery.




